Table of Abbreviations
Abbreviation Long Form
- ALC
- Alternate Level of Care
- FAO
- Financial Accountability Office
- LHIN
- Local Health Integration Network
- LOC
- Level of Care
- LTC
- Long-Term Care
- MLTC
- Ministry of Long-Term Care
1 | Executive Summary
Long-term care (LTC) homes provide accommodation to eligible Ontarians that require the availability of 24/7 nursing care and frequent assistance with daily activities. There are currently 626 LTC homes in Ontario that house over 78,000 residents.
LTC homes must be licensed by the Ministry of Long-Term Care (MLTC) and the ministry determines the number and location of long-term care beds in Ontario. LTC homes receive funding from the ministry through the long-term care homes program. Funding is provided based on the number of beds each LTC home has in operation and the types of services the LTC home provides.[1]
The Wait List and Wait Times for Long-Term Care Beds are Growing
In 2018-19 there were nearly 35,000 Ontarians on the wait list for a long-term care bed. The wait list for long-term care grew substantially from 2011-12 to 2018-19, increasing by approximately 78 per cent.
The growing LTC wait list has also led to increasing wait times for long-term care. From 2011-12 to 201819, the median time to placement (or wait time) for a long-term care bed increased from 99 days to 152 days.
Why Has the Wait List Increased?
High growth in the number of Ontarians aged 75 and over, combined with a lack of investment in new long-term care beds, have been the primary drivers of the growth in the long-term care wait list and wait times. Between 2011 and 2018, the number of long-term care beds in Ontario increased by only 0.8 per cent while the population of Ontarians aged 75 and over grew by 20 per cent.
Growth in elderly Ontarians has exceeded growth in the number of long-term care beds
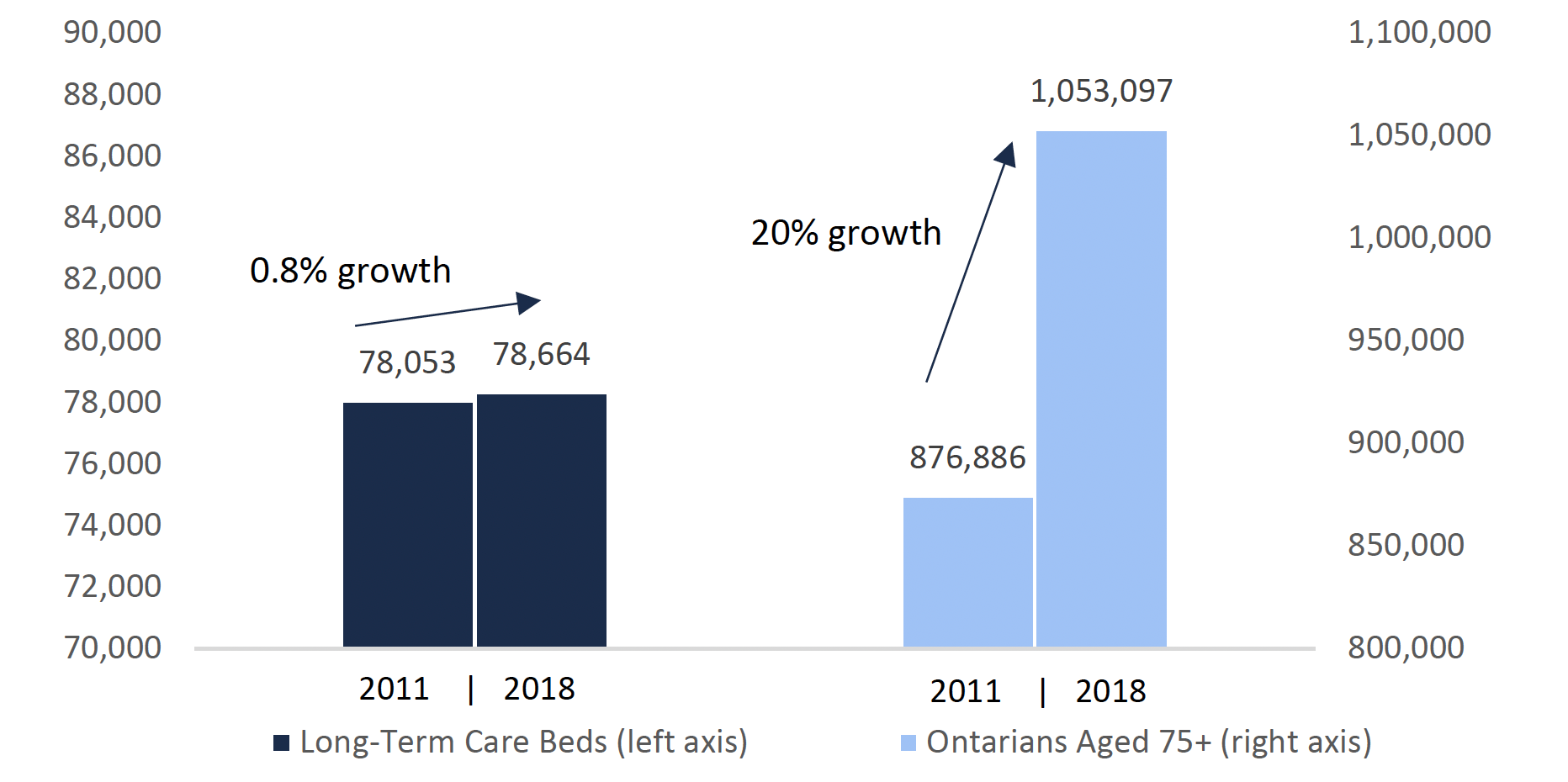
Source: Statistics Canada, Table 17-10-0005-01, Ministry of Finance, Ontario Population Projections 2018-2046, updated October 1, 2019, and information provided to the FAO by MLTC.
Accessible version
This chart shows the number of long-term care beds in 2011 and 2018 compared to the population of Ontarians aged 75 years and over in 2011 and 2018. The chart shows that the number of long-term care beds was 78,053 in 2011 and 78,664 in 2018 and the number of Ontarians aged 75 years and over was 876,886 in 2011 and 1,053,097 in 2018. The chart highlights the fact that the growth rate in long-term care beds from 2011 to 2018 was 0.8 per cent and the growth rate of Ontarians aged 75 years and over from 2011 to 2018 was 20 per cent.
Commitment to Increase LTC Beds
In July 2018, the Province announced its commitment to address wait times for long-term care by adding 15,000 new long-term care beds over five years (the LTC expansion).[2] In the 2019 Ontario Budget, the Province re-affirmed this commitment.[3] This is the largest new health sector spending commitment in the 2019 budget and is “a crucial part of the government’s priority to end hallway health care.”[4]
Timing of the LTC Expansion
As of the writing of this report, the Province has allocated 7,889 of the 15,000 new long-term care beds. Most of the 7,889 new beds were allocated in the 2018-19 fiscal year and should be in service by 2021-22. On October 1, 2019, the Province launched the application process for the remaining 7,111 beds with applications due by January 2020.
Overall, the FAO estimates that the Province must allocate the remaining beds by March 2021 if the remaining 7,111 LTC beds are to be in service by the end of the 2023-24 fiscal year. The following chart outlines the FAO forecast of when the new beds will be in service by fiscal year.
FAO projection of number of new LTC beds in service by fiscal year
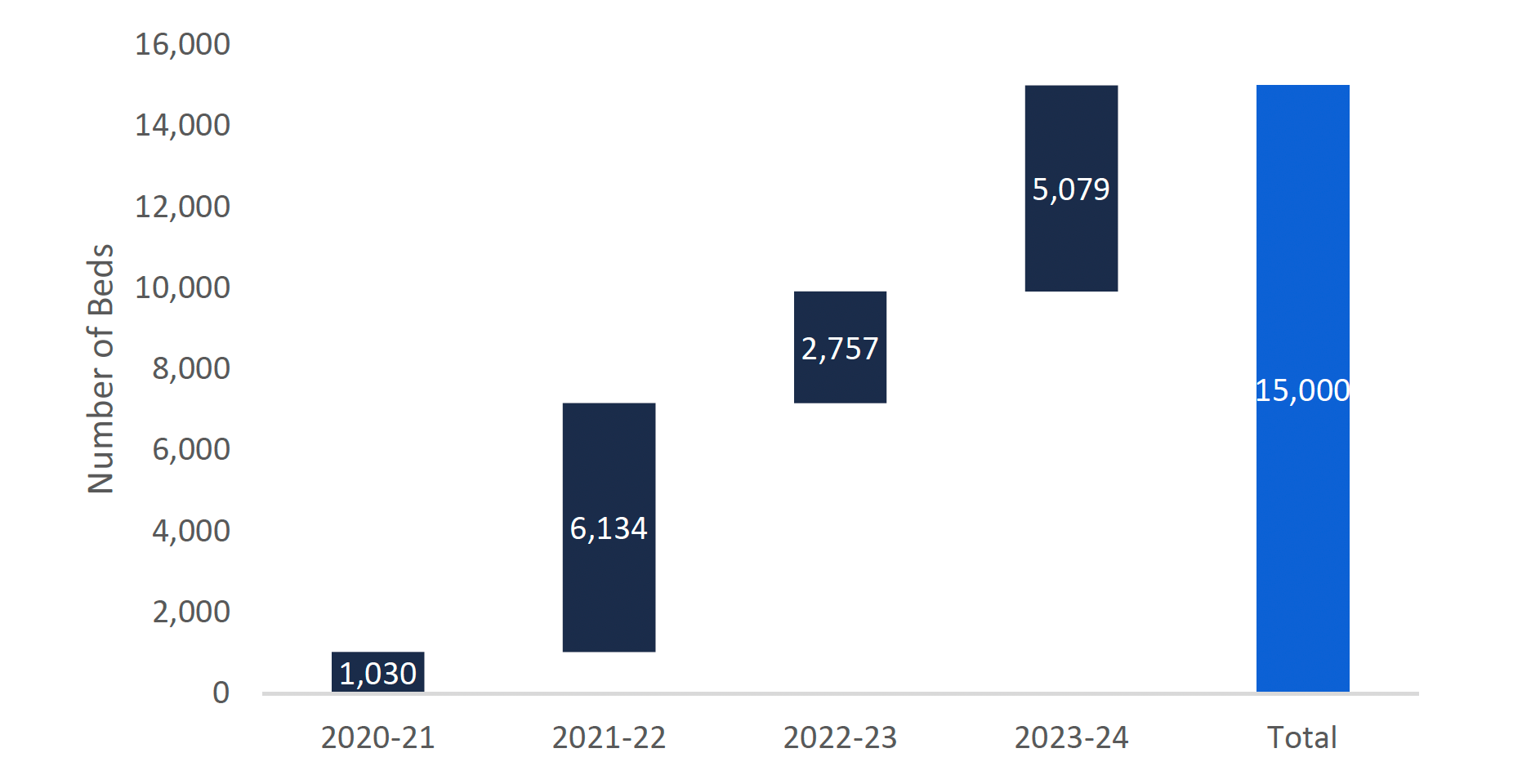
Source: FAO analysis of information provided by MLTC.
Accessible version
This chart shows the FAO’s projection of the number of new long-term care beds in service by fiscal year from 2020-21 to 2023-24. The chart shows that the number of new long-term care beds will be 1,030 in 2020-21, 6,134 in 2021-22, 2,757 in 2022-23, and 5,079 in 2023-24, showing 15,000 new long-term care beds in total.
Impact to the Province’s Budget Balance
The 15,000 new beds will not impact the Province’s budget balance until each bed comes into service.[5] Under the assumption that all 15,000 new LTC beds will be in operation by 2023-24, the FAO estimates that the LTC expansion will increase LTC homes program spending by a total of $1.7 billion over the next five years.
| ($ millions) | 2019-20 | 2020-21 | 2021-22 | 2022-23 | 2023-24 | Total |
|---|---|---|---|---|---|---|
| LTC homes program spending increase for 15,000 new LTC beds | 0 | 14 | 350 | 505 | 863 | 1,732 |
The annual cost will rise each year as more new beds come into service. Once all 15,000 new beds are in service, the LTC expansion will increase long-term care homes program spending by an ongoing annual amount of approximately $970 million.
The 15,000 new beds represent the first meaningful increase to the supply of long-term care beds in over 15 years and will result in LTC homes program spending growing much faster than the historical average. The FAO estimates that total LTC homes program spending will grow at an annual average of 5.4 per cent over the next five years, increasing from $4.3 billion in 2018-19 to $5.6 billion in 2023-24.
Wait List by 2023-24
Despite the significant increase in the number of long-term care beds, the FAO projects that the wait list for long-term care will increase by about 2,000 Ontarians over the next five years, from 34,900 in 2018-19 to approximately 36,900 Ontarians in 2023-24. The FAO projects that the wait list will peak at 40,200 Ontarians in 2020-21, an increase of about 5,300 from 2018-19, and will be reduced to 36,900 by 2023-24 as the new beds come into service.
LTC wait list projected to increase to 36,900 Ontarians by 2023-24
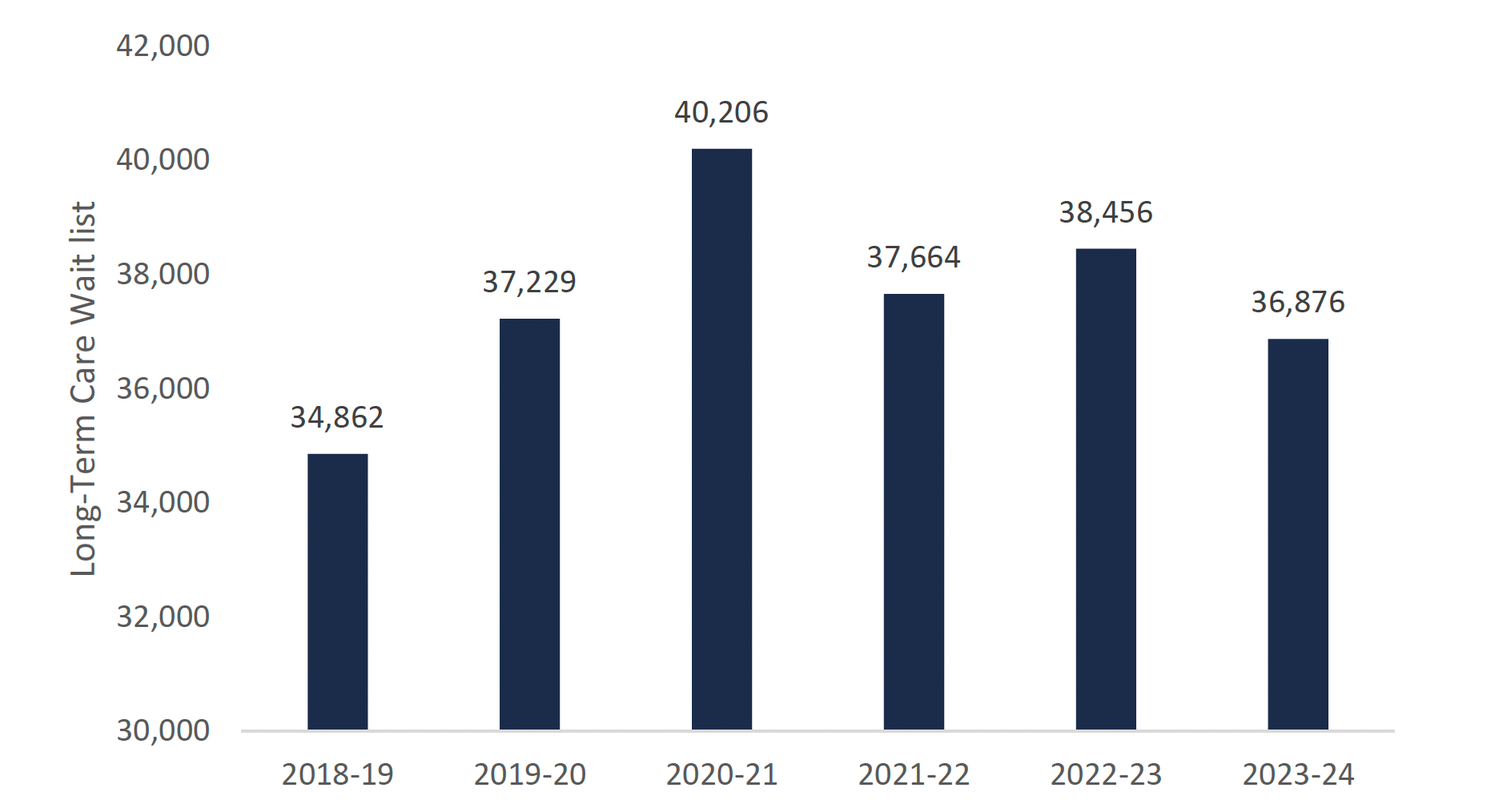
Source: FAO.
Accessible version
This chart shows the projected wait list for a long-term care bed from the 2018-19 fiscal year to the 2023-24 fiscal year. The chart shows that the number of people on the wait list for long-term care beds is 34,862 in 2018-19, 37,229 in 2019-20, 40,206 in 2020-21, 37,664 in 2021-22, 38,456 in 2022-23, and 36,876 in 2023-24.
The reason that the wait list for an LTC bed is projected to increase over the next five years, even with 15,000 new long-term care beds, is that the growth rate in the number of Ontarians aged 75 and over is projected to outpace the growth rate in LTC beds.
Wait Times by 2023-24
Despite the expected increase in the long-term care wait list over the next five years, the FAO projects a decrease in wait times by 2023-24. In 2018-19, the median time to placement for long-term care in Ontario was 152 days. Large numbers of new beds will not begin to come into service until the 2021-22 fiscal year. Therefore, the FAO projects time to placement will increase to 179 days by 2020-21. As the 15,000 new beds come into service, the FAO projects wait times will gradually decrease to 140 days by the 2023-24 fiscal year, reflecting a higher turnover of beds.
FAO projection for median time to placement (wait time) for a long-term care bed
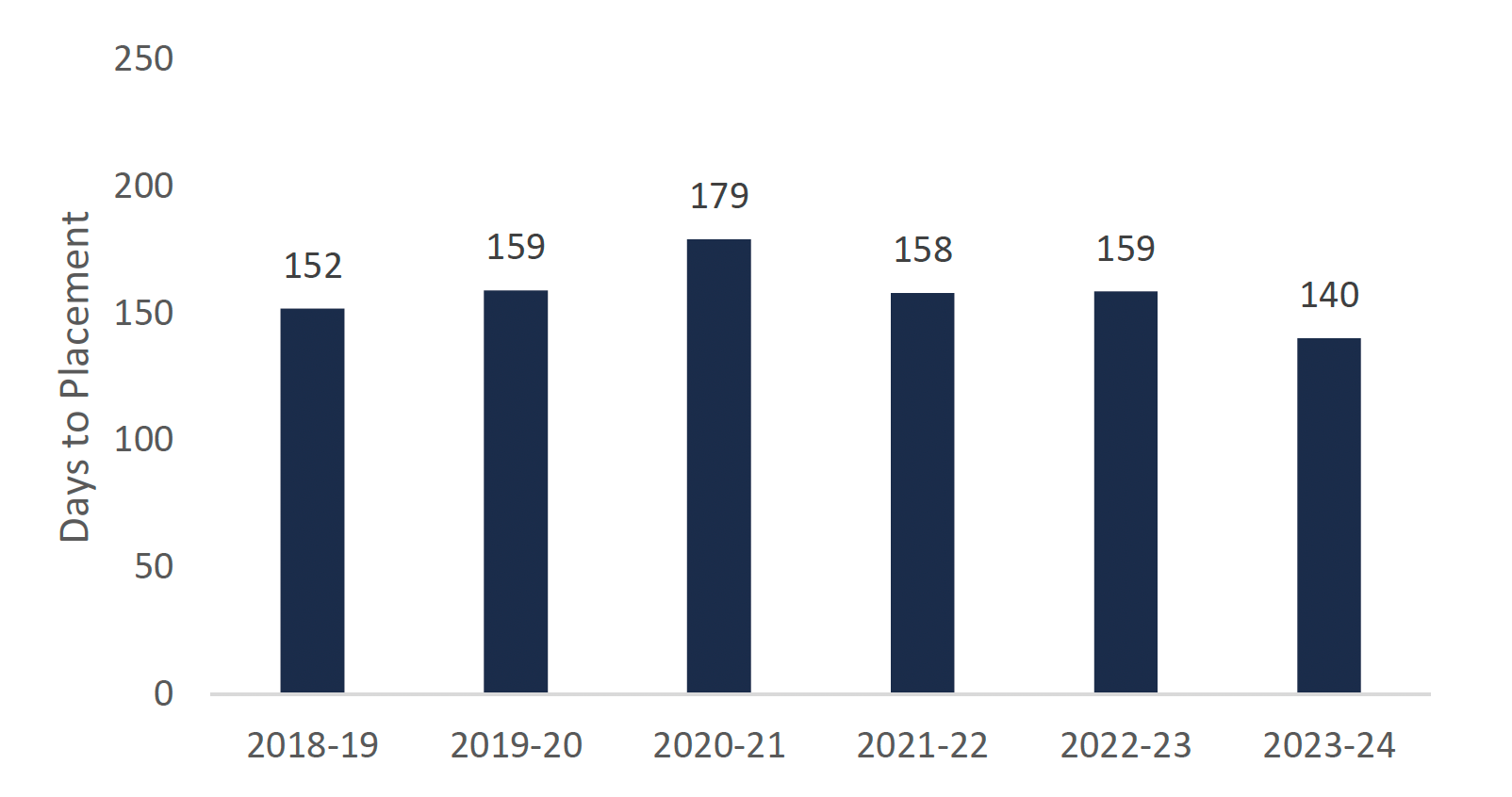
Source: FAO.
Accessible version
This chart shows a projection for the median time to placement (wait time) in days for a long-term care bed for each fiscal year between 2018-19 and 2023-24. The chart shows that the median wait time is 152 days for 2018-19, 159 days for 2019-20, 179 days for 2020-21, 158 days for 2021-22, 159 days for 2022-23, and 140 days for 2023-24.
55,000 More Ontarians Will Require an LTC Bed by 2033-34
After 2023-24, in order to maintain the projected wait list at approximately 36,900 Ontarians, the Province would need to create an additional 55,000 new long-term care beds by 2033-34. The need for 55,000 more long-term care beds to maintain the wait list results from higher projected demand growth for long-term care. From 2023-24 to 2033-34, the growth rate in the population of Ontarians aged 85 and older is projected to average 4.7 per cent, up from an average annual growth rate of 3.0 per cent from 2018-19 to 2023-24.
Will the LTC Expansion Help End Hallway Health Care?
“Hallway health care” refers to the estimated 1,000 patients waiting for a hospital bed in an unconventional space or emergency department stretcher on an average day in Ontario.
The wait time for a long-term care bed placement is a significant contributor to the problem of hallway health care in Ontario.[6] In 2017-18, there were approximately 6,300 hospital patients that spent time waiting for an LTC bed placement. Those patients occupied over 340,000 hospital bed days or about five per cent of all hospital bed days in Ontario.
As noted above, by 2023-24 the FAO is projecting a 2,000 person increase in the number of Ontarians on the long-term care wait list and a decrease in the median time to placement (from hospitals and the community) from 152 days in 2018-19 to 140 days in 2023-24. However, the FAO projects that the wait time for a long-term care bed will peak at 179 days in 2020-21. This implies that, in the absence of other health sector changes, the problem of hallway health care will get worse over the next two years.
By 2023-24, if all 15,000 new LTC beds have been opened, the wait time for an LTC bed is projected to decline to 140 days. If this improvement in LTC bed wait times also leads to patients spending less time in hospitals waiting for a long-term care bed, then, all else being equal, there could be an improvement in hallway health care by 2023-24 from the LTC bed expansion.
2 | Background and Context
Long-term care (LTC) homes provide accommodation to eligible Ontarians that require the availability of 24/7 nursing care and frequent assistance with daily activities. There are currently 626 LTC homes in Ontario that house over 78,000 residents. Most LTC residents are over the age of 75 and live with conditions that have compromised their health.
Long-term care homes can be for-profit, not-for-profit or municipal organizations which are governed by the Long-Term Care Homes Act, 2007. LTC homes must be licensed by the Ministry of Long-Term Care (MLTC) and the ministry determines the number and location of long-term care beds in Ontario. LTC homes receive funding from the ministry through the long-term care homes program. Funding is provided based on the number of beds each LTC home has in operation and the types of services the LTC home provides. In addition to funding provided by the ministry through the long-term care homes program, LTC homes also receive payments directly from residents.
The Wait List and Wait Times for LTC Beds are Growing
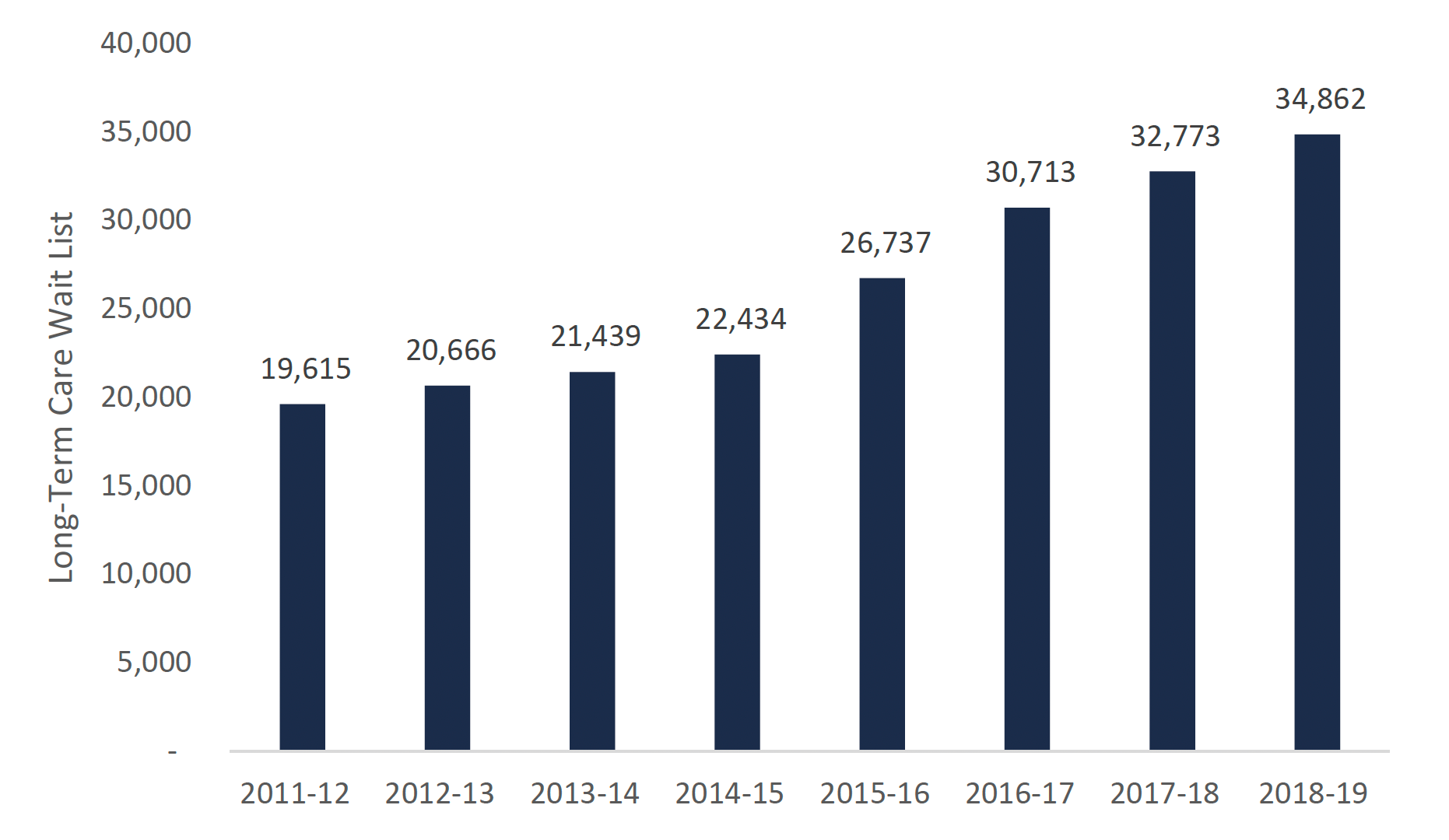
In 2018-19 there were nearly 35,000 Ontarians on the wait list for a long-term care bed. The wait list for long-term care has grown substantially since 2011-12, increasing by approximately 78 per cent over the last seven years.
Long-term care wait list
Source: Information provided to the FAO by MLTC.
Accessible version
This chart shows the number of Ontarians on the wait list for a long-term care bed from 2011-12 to 2018-19. The chart shows that the number of Ontarians on the wait list for a long-term care bed was 19,615 in 2011-12, 20,666 in 2012-13, 21,439 in 2013-14, 22,434 in 2014-15, 26,737 in 2015-16, 30,713 in 2016-17, 32,773 in 2017-18, and 34,862 in 2018-19.
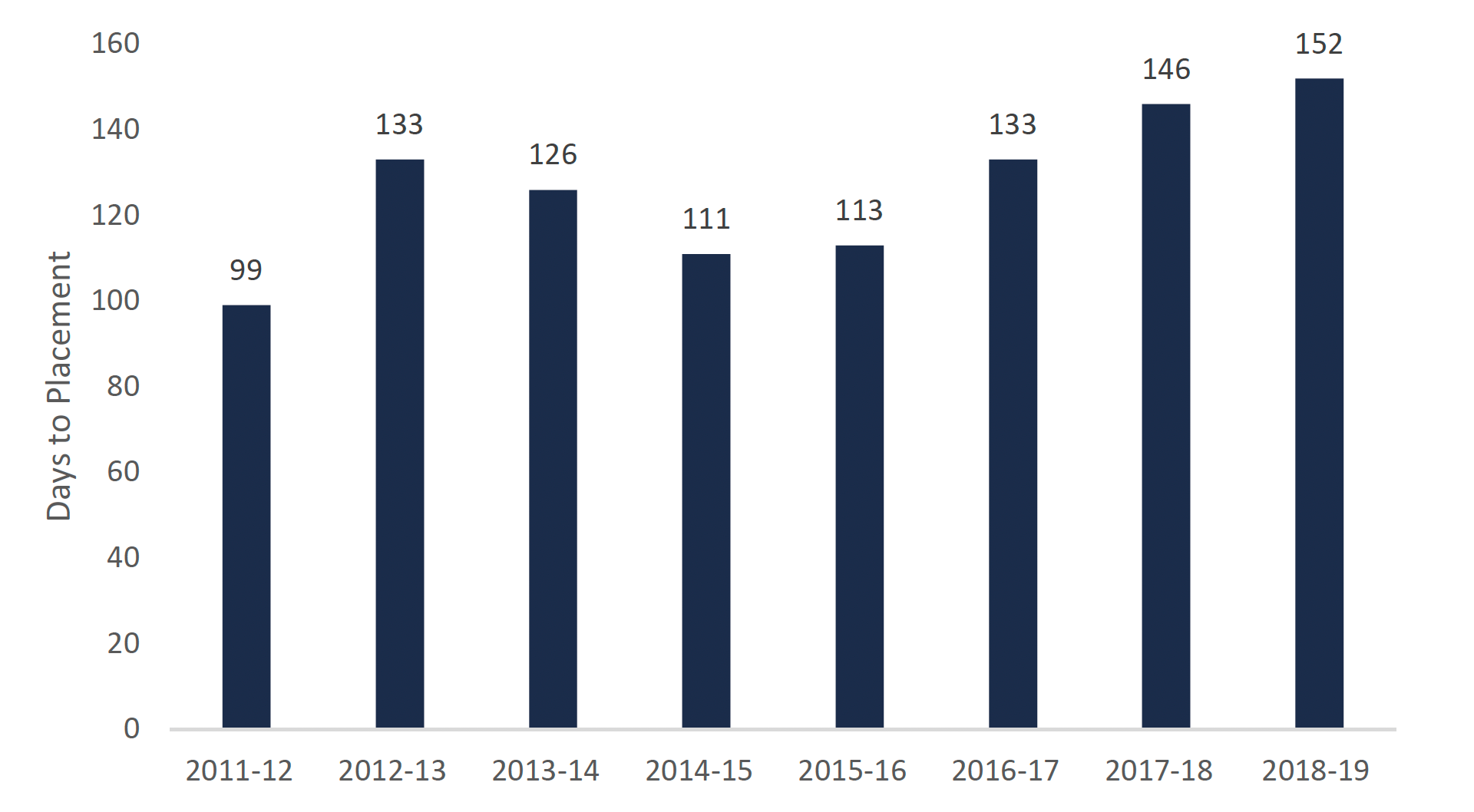
The growing LTC wait list has also led to increasing wait times for long-term care. From 2011-12 to 2018-19, the median time to placement (or wait time) for a long-term care bed increased from 99 days to 152 days.
Median time to placement (wait time) for a long-term care bed
Note: 2018-19 is an FAO estimate based on partial data on LTC placements in 2018-19.
Source: Information provided to the FAO by MLTC.
Accessible version
This chart shows the median time to placement (wait time) in days for a long-term care bed for each fiscal year between 2011-12 and 2018-19. The chart shows that the median wait time was 99 days in 2011-12, 133 days in 2012-13, 126 days in 2013-14, 111 days in 2014-15, 113 days in 2015-16, 133 days in 2016-17, 146 days in 2017-18, and 152 days in 2018-19.
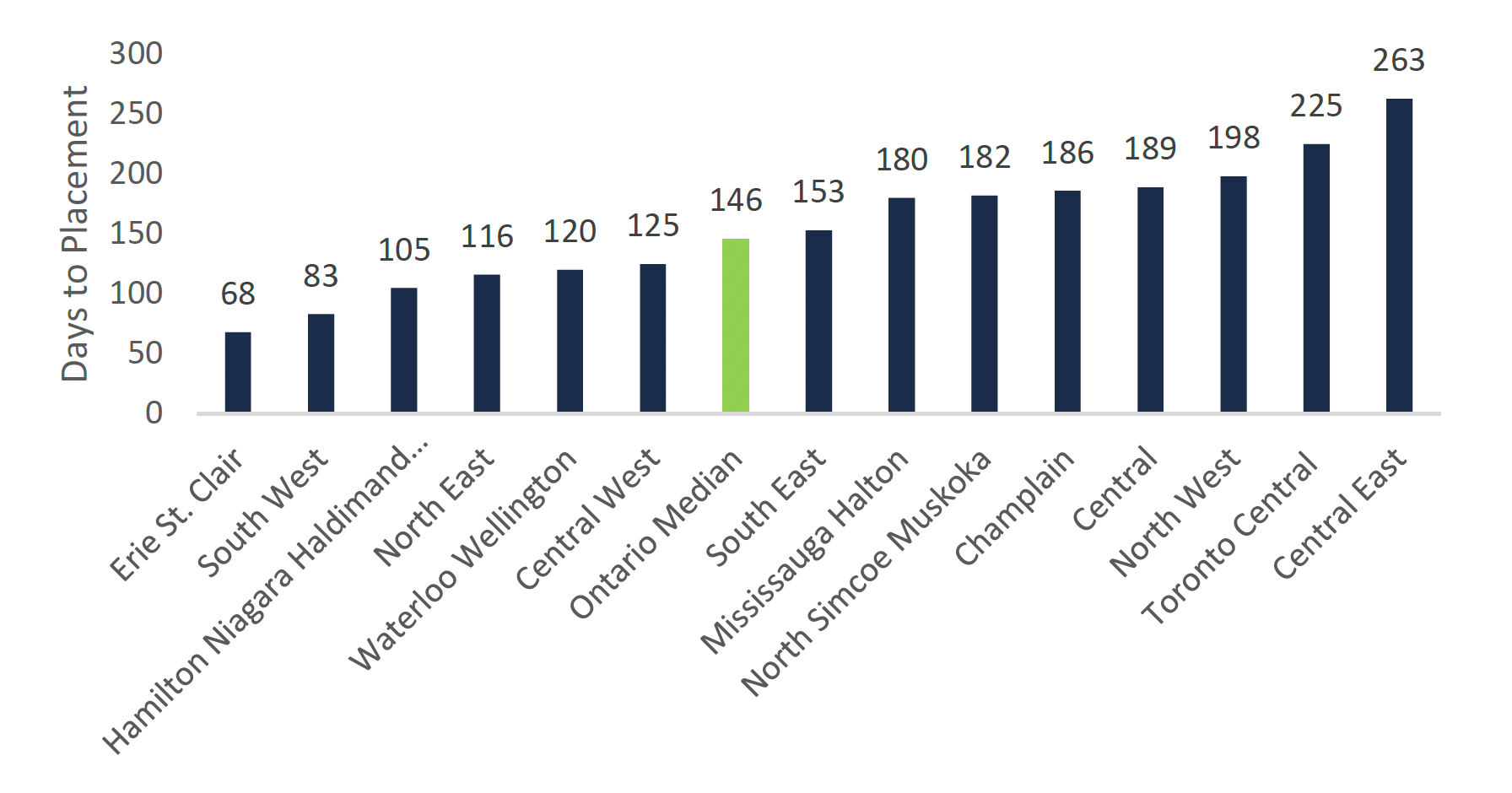
Wait times for long-term care vary significantly depending on where the individual is located in Ontario. The Province tracks wait times for long-term care geographically based on the Province’s 14 Local Health Integration Networks (LHINs).[7] In 2017-18, the median wait time for a long-term care bed ranged from 263 days in the Central East LHIN to 68 days in the Erie St. Clair LHIN.
Median time to placement (wait time) for a long-term care bed by LHIN (2017-18)
Source: Health Quality Ontario.
Accessible version
This chart shows the median time to placement in days for a long-term care bed by Local Health Integration Network (LHIN) in 2017-18. The chart shows that the time to placement for a long-term care bed in 2017-18 was 68 days in Erie St. Clair, 83 days in South West, 105 days in Hamilton Niagara Haldimand Brant, 116 days in North East, 120 days in Waterloo Wellington, 125 days in Central West, 153 days in South East, 180 days in Mississauga Halton, 182 days in North Simcoe Muskoka, 186 days in Champlain, 189 days in Central, 198 days in North West, 225 days in Toronto Central, and 263 days in Central East. The chart highlights the fact that the median time to placement across Ontario is 146 days.
Why Has the Wait List Increased?
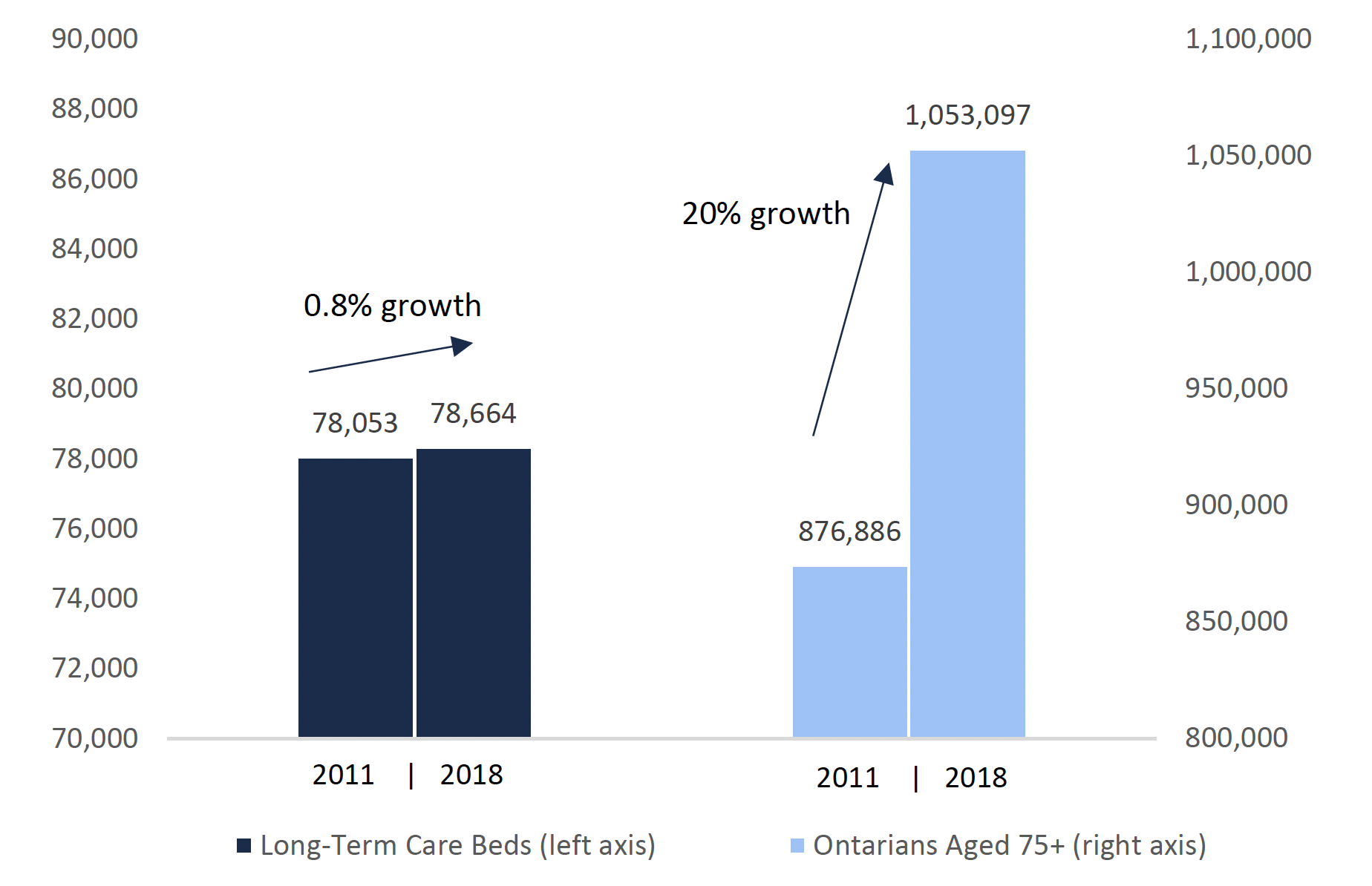
Over 80 per cent of long-term care residents are over the age of 75. High growth in the number of Ontarians aged 75 and over, combined with a lack of investment in new long-term care beds, have been the primary drivers of the growth in the long-term care wait list and wait times. Between 2011 and 2018, the number of long-term care beds in Ontario increased by only 0.8 per cent while the population of Ontarians aged 75 and over grew by 20 per cent.
Growth in elderly Ontarians has exceeded growth in the number of long-term care beds
Source: Statistics Canada, Table 17-10-0005-01, Ministry of Finance, Ontario Population Projections 2018-2046, updated October 1, 2019, and information provided to the FAO by MLTC.
Accessible version
This chart shows the number of long-term care beds in 2011 and 2018 compared to the population of Ontarians aged 75 years and over in 2011 and 2018. The chart shows that the number of long-term care beds was 78,053 in 2011 and 78,664 in 2018 and the number of Ontarians aged 75 years and over was 876,886 in 2011 and 1,053,097 in 2018. The chart highlights the fact that the growth rate in long-term care beds from 2011 to 2018 was 0.8 per cent and the growth rate of Ontarians aged 75 years and over from 2011 to 2018 was 20 per cent.
Commitment to Increase LTC Beds
In July 2018, the Province announced its commitment to address wait times for long-term care by adding 15,000 new long-term care beds over five years.[8] In the 2019 Ontario Budget, the Province re-affirmed this commitment.[9] This is the largest new health sector spending commitment in the 2019 budget and is “a crucial part of the government’s priority to end hallway health care.”[10]
Purpose and Structure of this Report
The purpose of this report is to analyze the Province’s commitment to create 15,000 new long-term care beds (the LTC expansion). The report explains how long-term care is funded by the Province and estimates the cost to the Province of the long-term care bed expansion commitment. The report then analyzes how the LTC expansion is expected to impact the wait list and wait times for LTC in the medium (5 years) and long-term (15 years). Finally, the report discusses the potential impact of the LTC expansion on the Province’s commitment to “end hallway health care”.
This report is structured as follows:
- Chapter 3 provides an overview of provincial spending on long-term care through the long-term care homes program.
- Chapter 4 presents the FAO’s estimate of the timing and cost of the LTC expansion.
- Chapters 5 and 6 project the impact of the LTC expansion on the wait list and wait times for long-term care over the medium and long-term.
- Lastly, Chapter 7 discusses how individuals waiting for long-term care impact hospital capacity and hallway health care.
Appendix C provides more information on the development of this report.
3 | Provincial Spending on Long-Term Care
In 2018-19, the Province spent $61.5 billion in the Ontario health sector, of which $4.3 billion, or 7 per cent, was spent in the long-term care homes program area.
LTC homes program represented 7 per cent of total health sector spending in 2018-19 ($ billions)
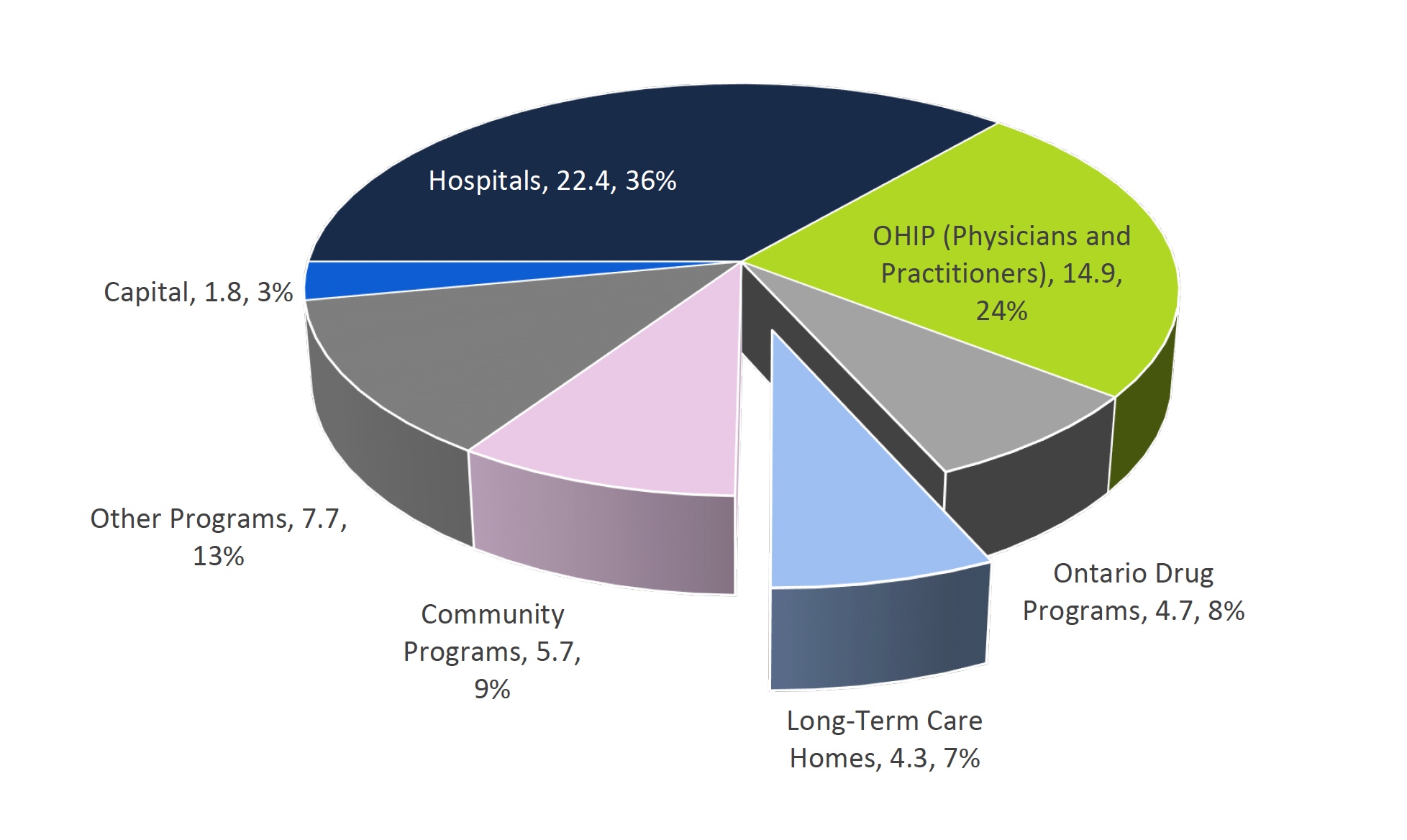
Source: 2018-19 Public Accounts of Ontario and information provided to the FAO by MLTC.
Accessible version
This pie chart breaks down the total spending on the Ontario health sector in 2018-19 in billions of dollars. The chart shows that $22.4 billion, or 36 per cent, was spent on hospitals, $14.9 billion, or 24 per cent, was spent on the Ontario Health Insurance Program (OHIP), $4.7 billion, or 8 per cent, was spent on Ontario Drug Programs, $5.7 billion, or 9 per cent, was spent on community programs, $7.7 billion, or 13 per cent was spent on other programs, and $1.8 billion, or 3 per cent, was spent on capital. The chart highlights that $4.3 billion, or 7 per cent, was spent on long-term care homes.
How Long-Term Care Spending Works
There are 626 long-term care homes in Ontario. LTC homes can be for-profit, not-for-profit, or municipally run organizations. LTC home operators receive funding from the Ministry of Long-Term Care, through the long-term care homes program, based on the number of beds in operation and the type of services provided. Long-term care home operators also receive payments from LTC residents. LTC residents are required to pay accommodation rates (co-payments) for long-term care which vary based on the type of accommodation they receive (e.g. basic, semi-private or private room).[11] A portion of the payments made by residents for accommodation is remitted back to the Province to offset some of the cost of the long-term care homes program.[12] In 2018-19, LTC residents offset $1.5 billion of the $5.8 billion cost of the long-term care homes program, for a net cost to the Province of $4.3 billion.
Most of the cost of the long-term care homes program (87 per cent) flows through a daily subsidy called the level of care (LOC) per diem payment, which is paid to long-term care home operators for each bed in operation. The LOC per diem payment covers the cost of nursing and personal care, basic accommodation, programs and support services, and raw food. The remaining 13 per cent cost of the LTC homes program flows through numerous supplementary funding streams that support specific ministry policy objectives. Supplementary funding streams include construction funding subsidies for new or redeveloped beds and funding for physiotherapy and behavioural supports. On average, each of the 78,664 beds in operation in 2018-19 cost the Province $149 per day. (See appendix A for more details on the LTC homes program spending categories.)
| Category | $ millions | % |
|---|---|---|
| Nursing and Personal Care | 2,919 | 50 |
| Program and Support Services | 279 | 5 |
| Raw Food | 268 | 5 |
| Basic Accommodation | 1,595 | 27 |
| Total LOC Per Diem | 5,062 | 87 |
| Supplementary Funding Programs | 764 | 13 |
| Total Cost of Long-Term Care Homes Program | 5,826 | 100 |
| Less: Resident Co-payments | – 1,537 | |
| Net Cost to Province of Long-Term Care Homes Program | 4,289 |
From 2011-12 to 2018-19 long-term care homes program spending grew by an annual average of 2.5 per cent, increasing from $3.6 billion in 2011-12 to $4.3 billion in 2018-19. Level of care per diem funding increased at an annual average of 2.1 per cent which is slightly higher than the rate of inflation over the same time period at 1.7 per cent. Supplementary funding increased at an annual average of 4.2 per cent. The high growth rate in supplementary funding was primarily driven by new funding streams introduced for physiotherapy and behavioural supports.
| $ billions | 2011-12 | 2012-13 | 2013-14 | 2014-15 | 2015-16 | 2016-17 | 2017-18 | 2018-19 | Average Annual Growth |
|---|---|---|---|---|---|---|---|---|---|
| Nursing and Personal Care | 2.5 | 2.5 | 2.6 | 2.6 | 2.7 | 2.7 | 2.8 | 2.9 | 2.3% |
| Program and Support Services | 0.2 | 0.2 | 0.2 | 0.3 | 0.3 | 0.3 | 0.3 | 0.3 | 2.4% |
| Raw Food | 0.2 | 0.2 | 0.2 | 0.2 | 0.2 | 0.2 | 0.3 | 0.3 | 3.6% |
| Basic Accommodation | 1.4 | 1.5 | 1.5 | 1.5 | 1.5 | 1.5 | 1.6 | 1.6 | 1.5% |
| Total LOC Per Diem | 4.4 | 4.4 | 4.5 | 4.6 | 4.7 | 4.8 | 4.9 | 5.1 | 2.1% |
| Supplementary Funding Programs | 0.6 | 0.6 | 0.7 | 0.7 | 0.7 | 0.7 | 0.7 | 0.8 | 4.2% |
| Total Cost of Long-Term Care Homes Program | 4.9 | 5.0 | 5.2 | 5.3 | 5.4 | 5.5 | 5.6 | 5.8 | 2.4% |
| Less: Resident Co-payments | -1.3 | -1.4 | -1.4 | -1.4 | -1.5 | -1.5 | -1.5 | -1.5 | 2.1% |
| Net Cost to Province of Long-Term Care Homes Program | 3.6 | 3.7 | 3.8 | 3.9 | 3.9 | 4.0 | 4.1 | 4.3 | 2.5% |
| Number of Beds | 78,053 | 77,444 | 77,862 | 78,006 | 78,340 | 78,357 | 78,517 | 78,664 | 0.1% |
4 | Timing and Cost of the LTC Expansion
Timing of the LTC Expansion
In July 2018, the Province announced its commitment to add 15,000 new long-term care beds over the next five years (the LTC expansion).[13] The process for building or redeveloping a long-term care bed in Ontario begins when the LTC home operator signs a development agreement with the Ministry of Long-Term Care. Once the development agreement is executed, the LTC operator must finance and construct the beds in accordance with the terms of the agreement. It takes approximately three years from the execution of a development agreement to when the first resident occupies a new bed.
As of the writing of this report, the Province has allocated 7,889 of the 15,000 new long-term care beds.[14] Most of the 7,889 new beds were allocated in the 2018-19 fiscal year and should be in service by 2021-22. On October 1, 2019, the Province launched the application process for the remaining 7,111 beds with applications due by January 2020. The ministry was not authorized to provide to the FAO its projection for when the remaining 7,111 beds will be in service,[15] although the ministry notes to potential applicants that they should consider the feasibility of completing projects by 2023 when applying.[16] Overall, the FAO estimates that the Province must allocate the remaining beds by March 2021 if the remaining 7,111 LTC beds are to be in service by the end of the 2023-24 fiscal year.[17]
The following chart outlines the FAO forecast of when the new beds will be in service by fiscal year. The forecast assumes that the 7,889 beds that have already been allocated will be in service three years from their allocation date.[18] The FAO forecast also assumes that the Province will receive enough applications so that the remaining 7,111 beds will be allocated by the end of the 2020-21 fiscal year and all 15,000 new beds will be in service by the end of the 2023-24 fiscal year.
FAO projection of number of new LTC beds in service by fiscal year
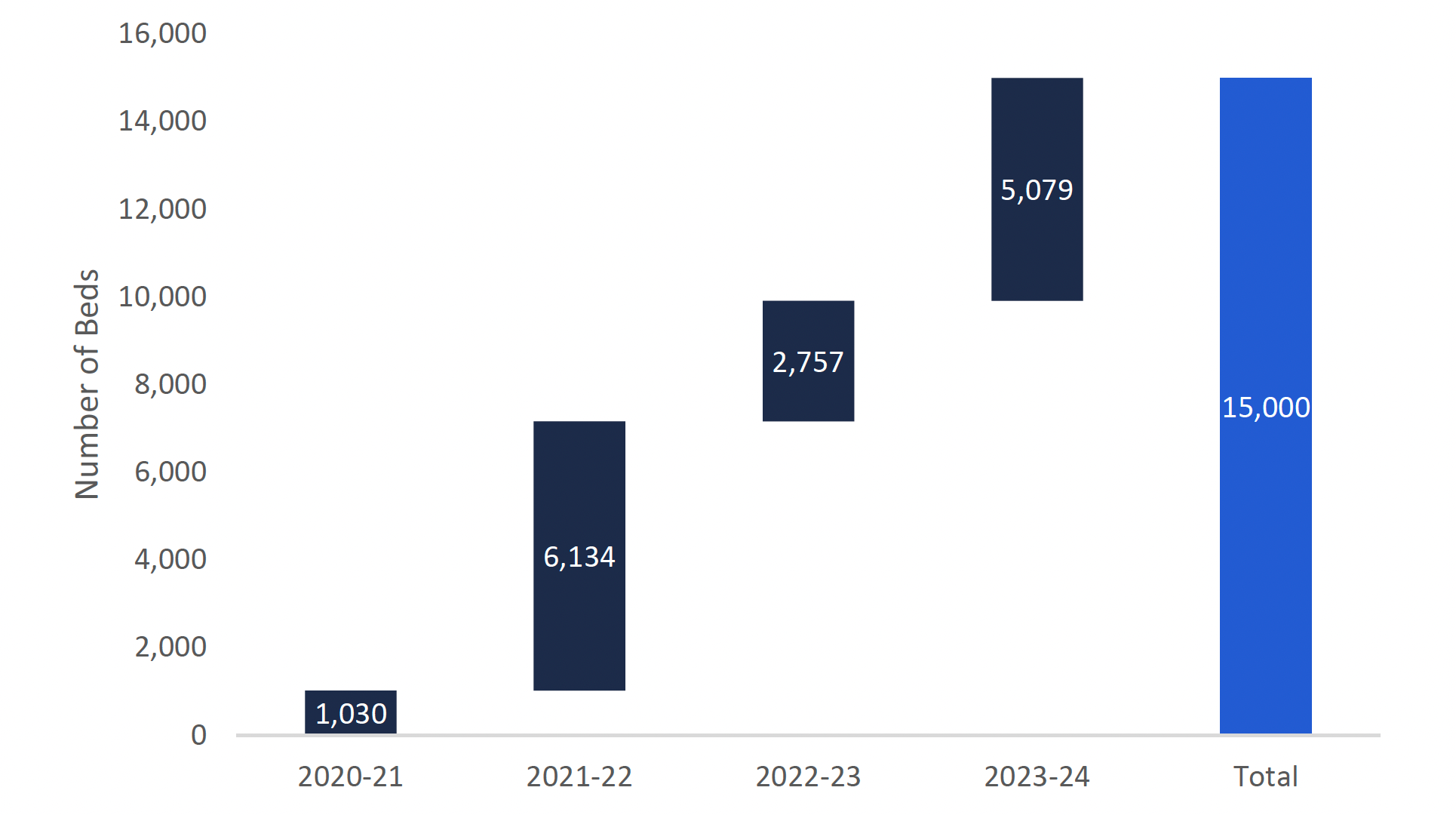
Source: FAO analysis of information provided by MLTC.
Accessible version
This chart shows the long-term care homes program expense from 2011-12 to 2023-24 in billions of dollars. The chart highlights that the average growth rate of the long-term care homes program expense from 2011-12 to 2018-19 was 2.5 per cent and the average growth rate of the long-term care homes program expense from 2019-20 to 2023-24 will be 5.4 per cent.
Impact to the Province’s Budget Balance
The 15,000 new beds will not impact the Province’s budget balance until each bed comes into service and begins to receive LOC per diem payments and supplementary funding.[19] The cost of constructing the new beds is subsidized by the Province after each new bed comes into service. Payment is made through the construction funding subsidy of the supplementary funding stream. As of 2019, a newly constructed bed that is in operation is eligible to receive a daily payment of between $18.03 and $23.03 over 25 years to cover the cost of construction.[20] In total, the FAO estimates the construction of the 15,000 new beds will cost the Province $2.0 billion (in 2019 dollars) over 25 years or about $135,000 (in 2019 dollars) per bed.[21]
Under the assumption that all 15,000 new LTC beds will be in operation by 2023-24, the FAO estimates that the LTC expansion will increase LTC homes program spending by a total of $1.7 billion over the next five years. This cost estimate includes the LOC per diem payments and supplementary funding paid by the Province (including construction funding subsidy payments). The annual cost will rise each year as more new beds come into service. Once all 15,000 new beds are in service, the LTC expansion will increase long-term care homes program spending by an ongoing annual amount of approximately $970 million.
| ($ millions) | 2019-20 | 2020-21 | 2021-22 | 2022-23 | 2023-24 | Total |
|---|---|---|---|---|---|---|
| LTC homes program spending increase for 15,000 new LTC beds | 0 | 14 | 350 | 505 | 863 | 1,732 |
Overall, the FAO estimates total LTC homes program spending will grow at an annual average of 5.4 per cent over the next five years, increasing from $4.3 billion in 2018-19 to $5.6 billion in 2023-24.[22] LTC homes program spending growth will begin to accelerate in the 2021-22 fiscal year as 6,134 new beds are projected to come into service in that year. The FAO estimates LTC homes program spending will grow at an annual average of 7.9 per cent from 2020-21 to 2023-24.
LTC homes program spending forecast ($ billions)
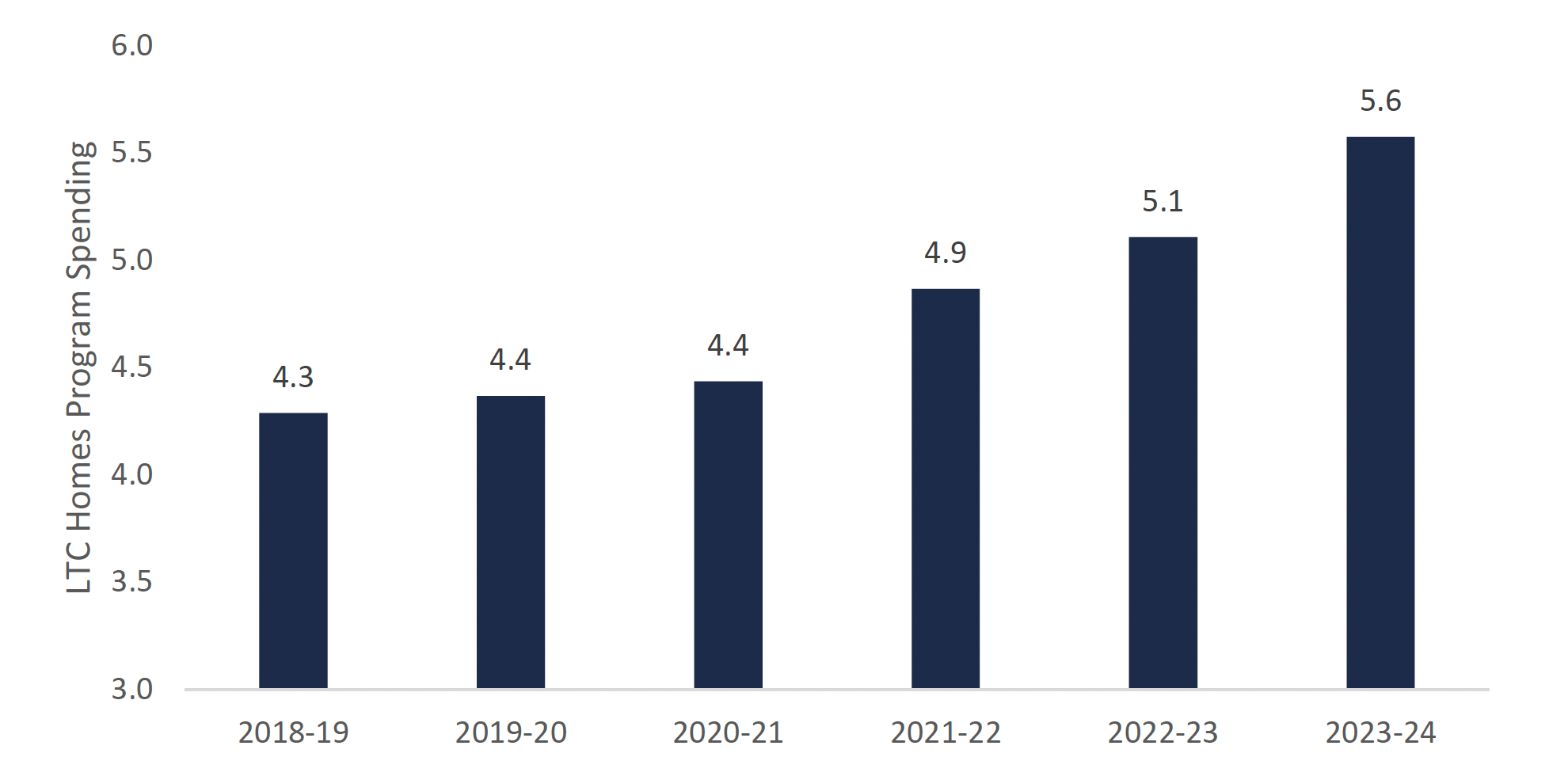
Source: FAO.
Accessible version
This chart shows the spending forecast of the long-term care homes program from 2018-19 to 2023-24 in billions of dollars. The chart shows a long-term care homes program expense of $4.3 billion in 2018-19, $4.4 billion in 2019-20, $4.4 billion in 2020-21, $4.9 billion on 2021-22, $5.1 billion in 2022-23, and $5.6 billion in 2023-24.
The 15,000 new beds represent the first meaningful increase to the supply of long-term care beds in over 15 years and will result in LTC homes program spending growing much faster than the historical average. For reference, from 2011-12 to 2018-19, long-term care homes program spending increased by an annual average of only 2.5 per cent.
LTC homes program spending annual growth rate will increase significantly over the next five years ($ billions)
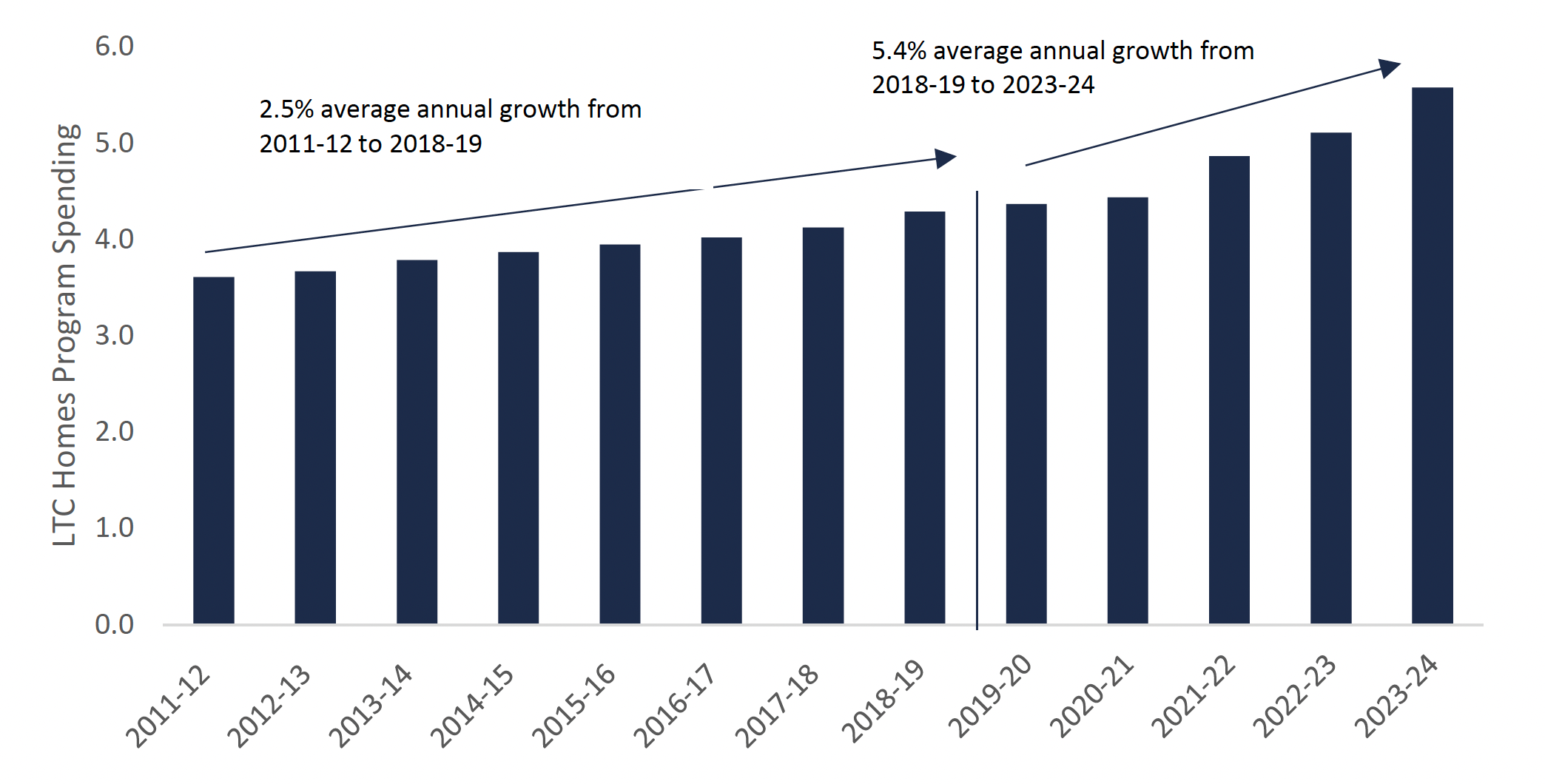
Source: Information provided to the FAO by MLTC and FAO.
Accessible version
This chart shows the long-term care homes program expense from 2011-12 to 2023-24 in billions of dollars. The chart highlights that the average growth rate of the long-term care homes program expense from 2011-12 to 2018-19 was 2.5 per cent and the average growth rate of the long-term care homes program expense from 2019-20 to 2023-24 will be 5.4 per cent.
5 | Effect on LTC Wait Times
Total Number of LTC Beds by 2023-24
Based on the assumptions in the previous chapter on the timing of the LTC expansion, the 15,000 new long-term care beds will increase the supply of long-term care spaces in Ontario from 78,700 in 2018-19 to approximately 93,700 in 2023-24. The growth in the number of LTC beds will begin to accelerate in the 2021-22 fiscal year as approximately 6,134 new beds are projected to be completed in that year.
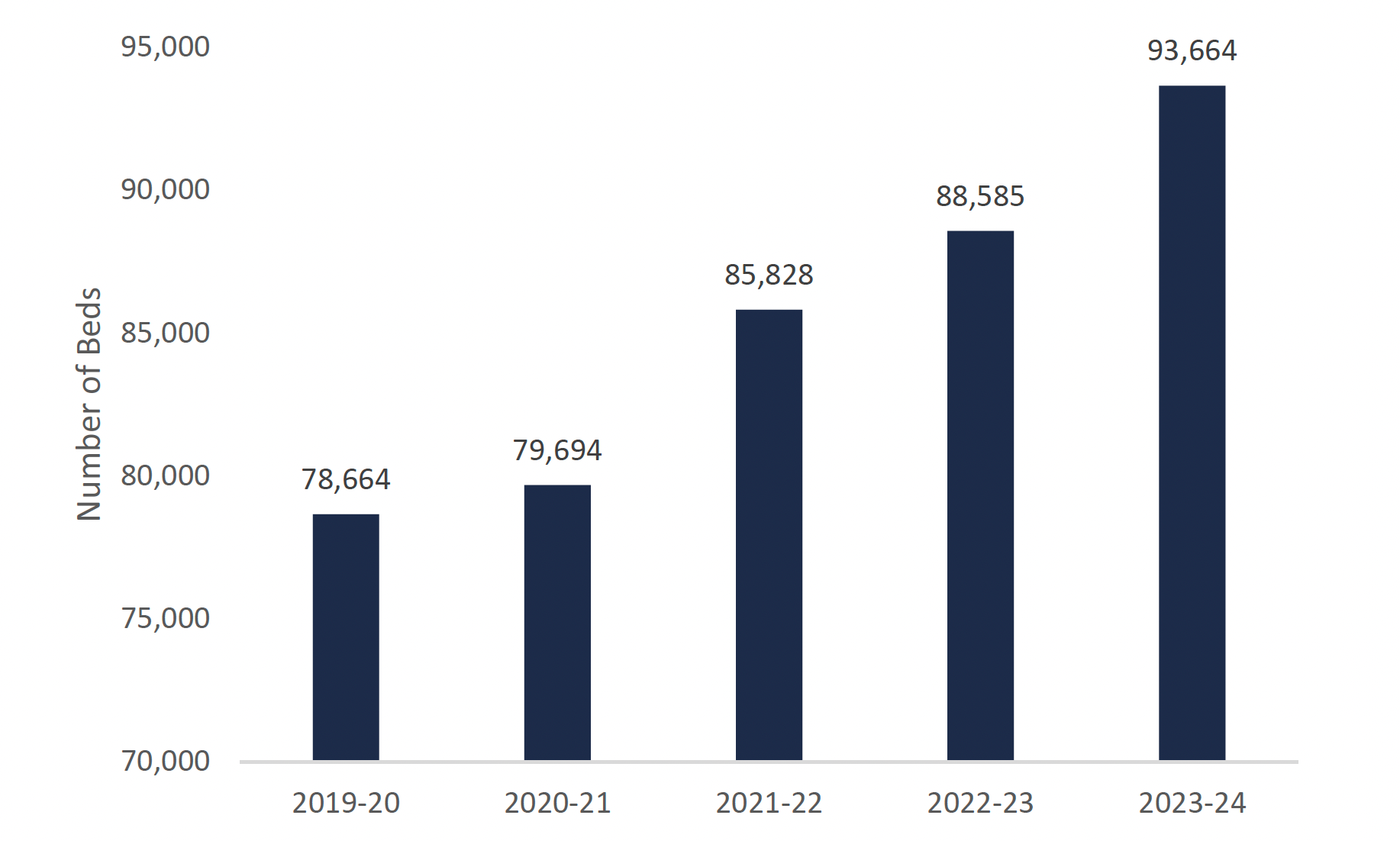
Projected number of long-term care beds in Ontario
Source: FAO analysis of information provided by MLTC.
Accessible version
This chart shows the projected number of long-term care beds in Ontario from 2019-20 to 2023-24. The chart shows that the number of long-term care beds is 78,664 in 2019-20, 79,694 in 2020-21, 85,828 in 2021-22, 88,585 in 2022-23, and 93,664 in 2023-24.
Wait List by 2023-24
Despite the significant increase in the number of long-term care beds, the FAO projects that the wait list for long-term care will increase by about 2,000 Ontarians over the next five years, from 34,900 in 2018-19 to approximately 36,900 Ontarians in 2023-24.[23] The FAO projects that the wait list will peak at 40,200 Ontarians in 2020-21, an increase of about 5,300 from 2018-19, and will be reduced to 36,900 by 2023-24 as the new beds come into service.
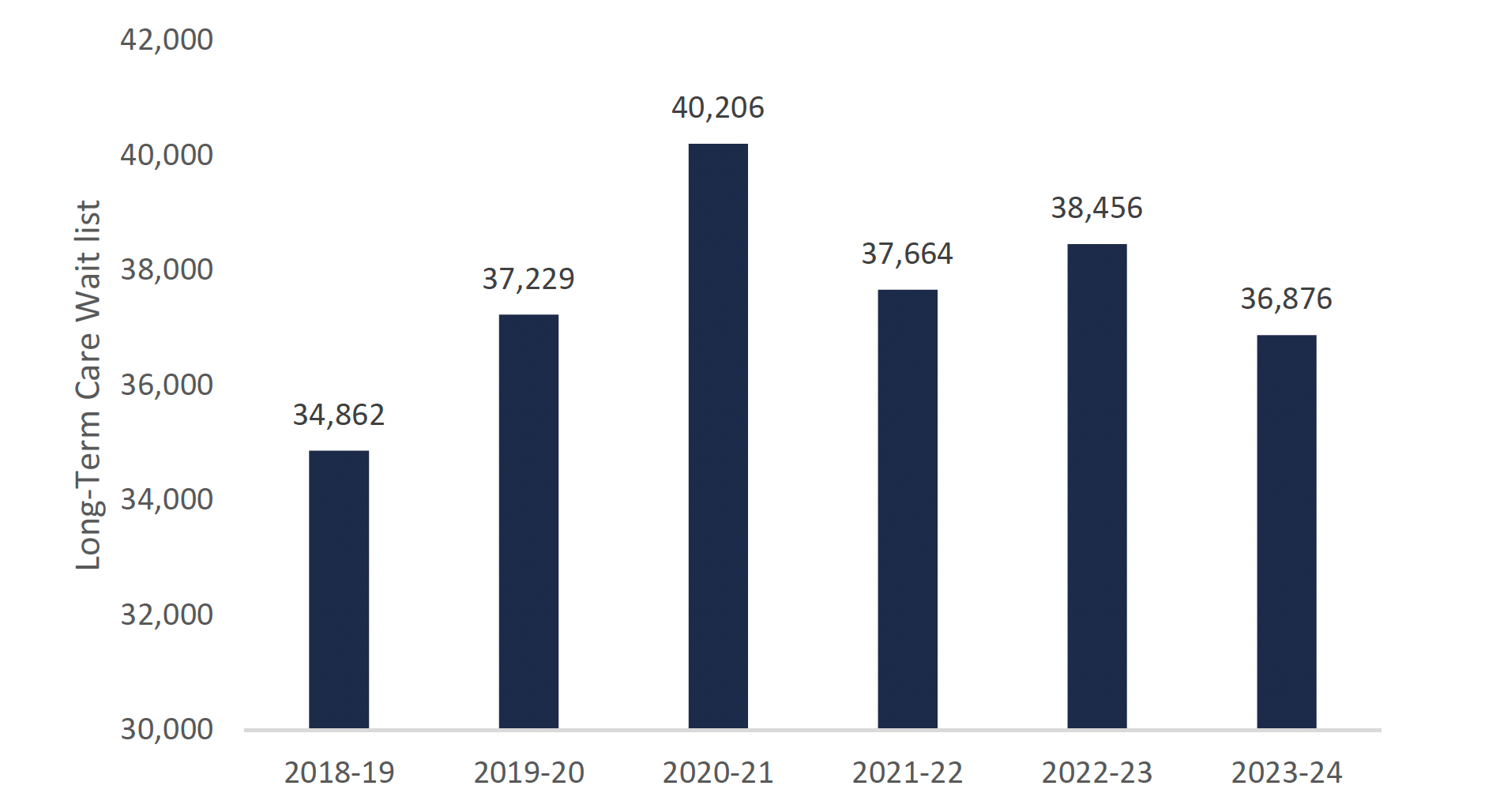
LTC wait list projected to increase to 36,900 Ontarians by 2023-24
Source: FAO.
Accessible version
This chart shows the projected wait list for a long-term care bed from the 2018-19 fiscal year to the 2023-24 fiscal year. The chart shows that the number of people on the wait list for long-term care beds is 34,862 in 2018-19, 37,229 in 2019-20, 40,206 in 2020-21, 37,664 in 2021-22, 38,456 in 2022-23, and 36,876 in 2023-24.
The reason the wait list for an LTC bed is projected to increase (even with 15,000 more LTC beds) is that the number of Ontarians in need of a long-term care bed placement (or LTC demand) is expected to increase by 17,000, outpacing the 15,000 new beds. The large increase in LTC demand over the next five years is primarily due to an expected accelerated growth rate in the number of elderly Ontarians. From 2018-19 to 2023-24, the number of Ontarians aged 75 and over is projected to grow by an annual average of 4.3 per cent.[24] For comparison, from 2013-14 to 2018-19, the number of Ontarians aged 75 and over grew at an annual average rate of only 2.8 per cent.[25] Over that time period, the wait list for long-term care beds increased by 13,000 Ontarians.
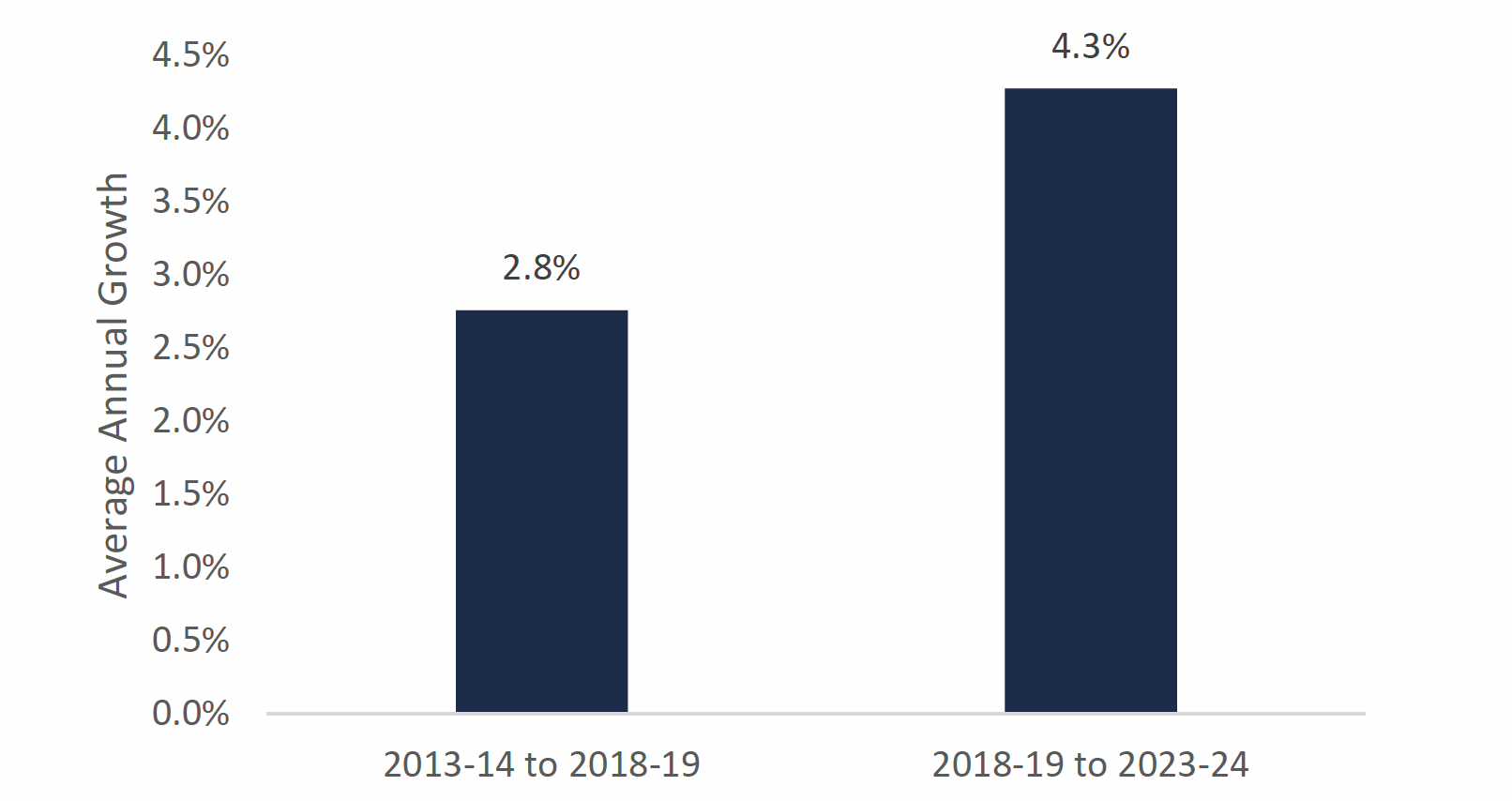
Growth in Ontarians aged 75 and over will accelerate over the next five years
Source: Statistics Canada, Table 17-10-0005-01 and Ministry of Finance, Ontario Population Projections 2018-2046, updated October 1, 2019.
Accessible version
This chart shows average annual growth rate of Ontarians aged 75 and over from the years 2013-14 to 2018-19 compared to the years 2018-19 to 2023-24. The chart highlights that the average annual growth rate of Ontarians aged 75 years and over was 2.8 per cent from 2013-14 to 2018-19 and 4.3 per cent from 2018-19 to 2023-24.
Wait Times by 2023-24
Despite the expected increase in the long-term care wait list over the next five years, the FAO projects a decrease in wait times by 2023-24. In 2018-19, the median time to placement for long-term care in Ontario was 152 days. As large numbers of new beds will not begin to come into service until the 2021-22 fiscal year, the FAO projects time to placement will increase to 179 days by 2020-21. As the new beds come into service, the FAO projects wait times will gradually decrease to 140 days by the 2023-24 fiscal year.
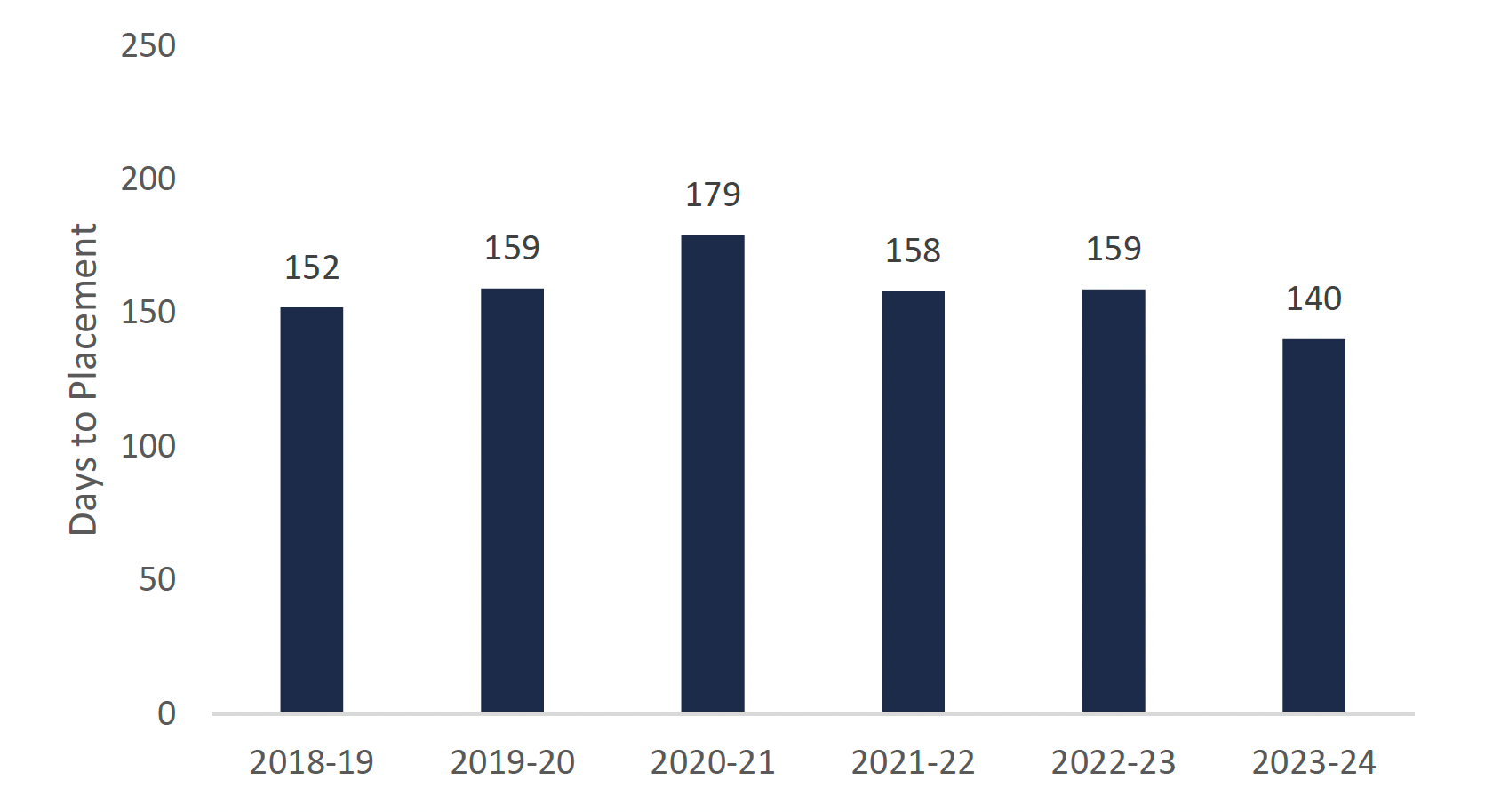
FAO projection for median time to placement (wait time) for a long-term care bed
Source: FAO.
Accessible version
This chart shows a projection for the median time to placement (wait time) in days for a long-term care bed for each fiscal year between 2018-19 and 2023-24. The chart shows that the median wait time is 152 days for 2018-19, 159 days for 2019-20, 179 days for 2020-21, 158 days for 2021-22, 159 days for 2022-23, and 140 days for 2023-24.
The reason the wait list is expected to increase while wait times are expected to decline reflects the fact that with 15,000 more long-term care beds in operation there will be a higher turnover of beds. Approximately 28 per cent of long-term care beds turnover each year and from 2013-14 to 2017-18 there was an average of 21,000 long-term care placements each year. With the addition of 15,000 new beds, approximately 4,200 more beds will turnover each year, which the FAO estimates will result in reduced wait times despite the growing wait list.
Regional Impact
The Province has indicated that it will prioritize the allocation of new LTC beds to areas where the beds will have the greatest impact on wait times and hallway health care.[26] As noted previously, wait lists and time to placement vary significantly by LHIN geographic region. The variation is due to differences in the supply/demand balance, demographics, and the availability of alternatives to long-term care such as community-based care.[27]
To date, the Ministry of Long-Term Care has allocated 7,889 of the 15,000 new bed commitment. For the most part, the 7,889 new beds have been allocated to the LHIN regions with the longest wait lists and/or wait times. For example, the six LHIN regions that have received the most new beds also have the longest wait lists.
| LHIN | Number of new beds allocated | LTC wait list (rank) |
Median time to placement (rank) |
|---|---|---|---|
| Central East | 1,095 | 7,080 (1) | 263 (1) |
| Hamilton Niagara Haldimand Brant | 1,080 | 3,027 (4) | 105 (12) |
| Toronto Central | 1,069 | 2,633 (5) | 225 (2) |
| Central | 1,064 | 4,948 (2) | 189 (4) |
| Champlain | 751 | 3,356 (3) | 186 (5) |
| Mississauga Halton | 649 | 2,300 (6) | 180 (7) |
| North Simcoe Muskoka | 401 | 1,959 (8) | 182 (6) |
| South East | 400 | 1,400 (11) | 153 (8) |
| North East | 384 | 2,040 (7) | 116 (11) |
| South West | 291 | 1,769 (9) | 83 (13) |
| Central West | 266 | 997 (12) | 125 (9) |
| North West | 201 | 817 (13) | 198 (3) |
| Waterloo Wellington | 186 | 1,726 (10) | 120 (10) |
| Erie St. Clair | 52 | 810 (14) | 68 (14) |
Looking forward, the FAO is unable to project the overall impact of the 15,000 LTC bed expansion on the wait list or time to placement by LHIN region as the remaining 7,111 beds have yet to be allocated.
Wait Time Targets and Benchmarks
The Ministry of Long-Term Care does not have a target for the wait list or wait times for a long-term care bed, or a benchmark (such as another jurisdiction) to compare against changes to the wait list or wait times.
Health Quality Ontario (HQO)[28] publicly reports on 12 indicators or measures of the quality of long-term care. However, only five of the indicators currently have targets or benchmarks. While median time to placement (or wait times) is an indicator measured by HQO, and reported publicly, HQO has not identified an appropriate target or benchmark for LTC wait times.[29]
Compared to British Columbia and Alberta, Ontario has significantly longer wait times for a long-term care bed. In British Columbia, there are 28,000 long-term care beds with a wait list of about 1,400 people and a median time to placement (wait time) of 12 days. In addition, some provinces do have wait time targets. For example, Alberta has a target of placing 65 per cent of patients into continuing care[30] within 30 days.[31] In 2017-18, Alberta fell short of the target, placing only 52 per cent of clients within the 30-day window.[32] By comparison, less than three per cent of long-term care homes in Ontario place 50 per cent of clients within 30 days.
6 | Long-Term Implications
High Growth in Elderly Ontarians Will Continue Past 2023-24
Growth in the number of Ontarians aged 75 and over is the primary driver of long-term care demand in Ontario. Over 80 per cent of Ontarians in long-term care are over the age of 75. However, as a person ages, the likelihood they will be in provincially funded long-term care increases. For example, an individual aged 85 or older is over seven times more likely to be in long-term care than a 75-year-old.[33]
As noted in chapter 5, the growth rate of the Ontario population aged 75 and over is projected to accelerate to 4.3 per cent annual growth from 2018-19 to 2023-24 compared to 2.8 per cent over the prior five-year period. This accelerated growth rate is projected to continue for the 10-year period from 2023-24 to 2033-34 at 4.2 per cent average annual growth.
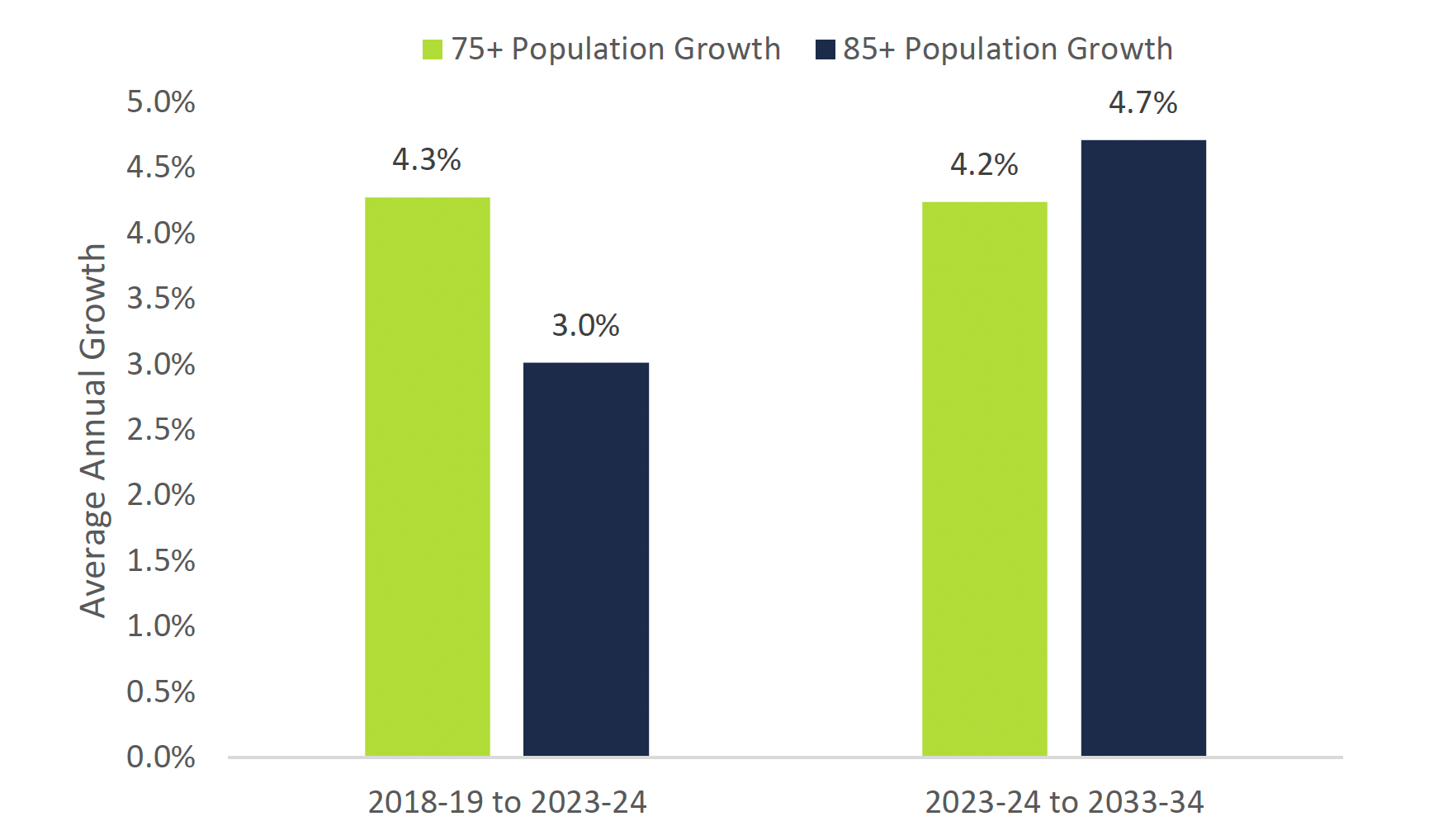
More importantly, the growth rate of Ontarians over the age of 85 is projected to increase significantly. From 2023-24 to 2033-34, the growth rate in the population of Ontarians aged 85 and older is projected to average 4.7 per cent, up from an average annual growth rate of 3.0 per cent from 2018-19 to 2023-24.
Growth in Ontarians aged 85 and over will accelerate over the long-term
Source: FAO analysis of Ministry of Finance, Ontario Population Projections 2018-2046, updated October 1, 2019.
Accessible version
This chart shows a comparison between the average annual growth rate of Ontarians aged 75 years and over and 85 years and over from 2018-19 to 2023-24 and from 2023-24 to 2033-34. The chart shows that the average annual growth rate of Ontarians aged 75 years and over is 4.3 per cent from 2018-19 to 2023-24 and 4.2 per cent from 2023-24 to 2033-34. The chart also shows that the average annual growth rate of Ontarians aged 85 years and over is 3.0 per cent from 2018-19 to 2023-24 and 4.7 per cent from 2023-24 to 2033-34.
55,000 More Ontarians Will Require an LTC Bed by 2033-34
Based on the projections for Ontario population growth and population aging noted above, the FAO forecasts that 55,000 more Ontarians will require a long-term care placement in 2033-34 compared to 2023-24.[34] Therefore, to maintain the projected wait list in 2023-24 at approximately 36,900 Ontarians, the Province would need to add 55,000 new long-term care beds by 2033-34 and ensure that all existing beds stay in service.[35] This would result in a total supply of long-term care beds in 2033-34 of 148,700, up from a projected 93,700 LTC beds in 2023-24.
7 | Impact of the LTC Expansion on Hallway Health Care
LTC Bed Wait Times Contribute to Hallway Health Care
“Hallway health care” refers to the estimated 1,000 patients waiting for a hospital bed in an unconventional space or emergency department stretcher on an average day in Ontario. Hallway health care is a symptom of capacity pressures in the Ontario health sector resulting from Ontario not having the appropriate mix of services and beds throughout the health system.[36]
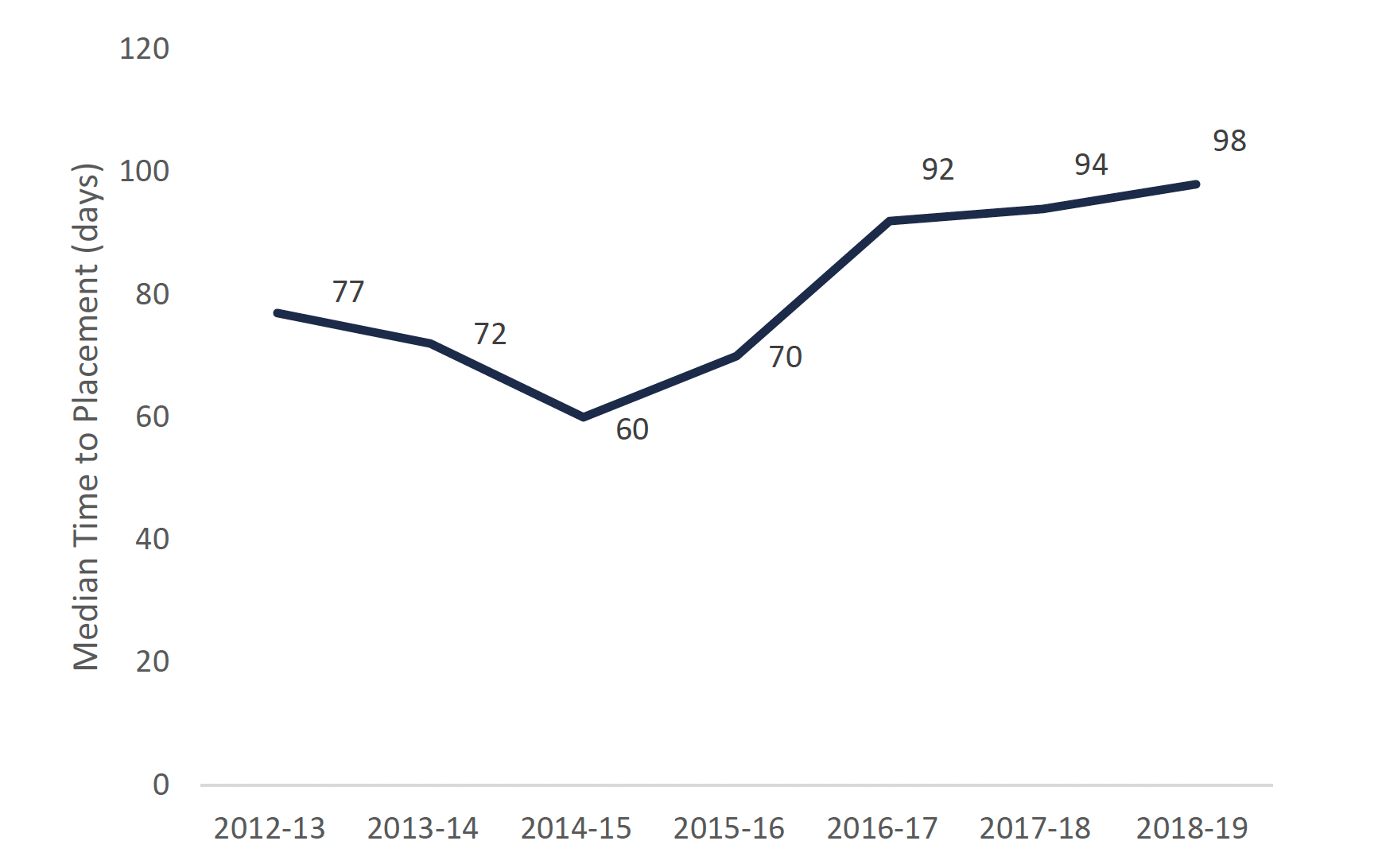
The wait time for a long-term care bed placement is a significant contributor to the problem of hallway health care in Ontario. Approximately 24 per cent of long-term care residents are placed from hospitals. In 2018-19, the median time to placement (or wait time) for a long-term care bed for residents from hospitals was 98 days. From 2012-13 to 2018-19 the wait time for a long-term care bed for patients waiting in hospitals increased by 27 per cent, from 77 days to 98 days. Overall, increasing wait times for hospital patients requiring a long-term care bed occupies valuable hospital capacity and is detrimental to patients’ health and well-being.[37]
Median time to long-term care bed placement for patients waiting in hospitals
Source: Health Quality Ontario and information provided to the FAO by MLTC.
Accessible version
This chart shows the median time to placement in days for a long-term care bed for patients waiting in hospitals from 2012-13 to 2018-19. The chart shows that the median time to placement was 77 days in 2012-13, 72 days in 2013-14, 60 days in 2014-15, 70 days in 2015-16, 92 days in 2016-17, 94 days in 2017-18, and 98 days in 2018-19.
Patients discharged to long-term care homes from hospitals represent about two per cent of all hospital patients. However, due to long LTC wait times, those patients represent one-third of the alternate level of care (ALC) days in Ontario. A patient is designated as ALC when they no longer need care in hospital but continue to occupy a hospital bed while waiting to go elsewhere like a long-term care home or rehabilitation facility. In November 2018, over 4,600 of the Province’s 34,000 hospital beds were occupied by ALC patients waiting to go elsewhere.[38]
ALC patients waiting for a long-term care bed spend much more time occupying a hospital bed than other ALC patients. On average, ALC patients that are transferred to a long-term care bed spend 69 days in the hospital, with 54 of those days designated as ALC. On the other hand, all other ALC patients spend an average of 29 days in the hospital, with only 15 of those days designated as ALC.
| Acute Care Days | ALC Days | Total average length of stay in hospital | |
|---|---|---|---|
| ALC patients waiting for a long-term care bed | 15 | 54 | 69 |
| All other ALC patients | 14 | 15 | 29 |
ALC Patients in Hospitals More Costly than Residents in Long-Term Care
In 2017-18, there were approximately 6,300 hospital patients designated as ALC that spent time waiting for an LTC placement. Those patients occupied over 340,000 hospital bed days or about five per cent of all hospital bed days in Ontario. Each day a patient remains in hospital designated as ALC while waiting for an LTC bed costs the Province approximately $500 more than if the patient were in a long-term care home bed. Therefore, in 2017-18 ALC patients waiting in hospitals for long-term care beds cost the Province approximately $170 million.
Will the LTC Expansion Help End Hallway Health Care?
The Province has indicated that it will prioritize the allocation of new long-term care beds to areas where the beds will have the greatest impact on wait times and hallway health care. For the most part, the 7,889 currently allocated beds are being placed in areas with the longest wait lists and the highest number of hospital bed days being occupied by patients waiting for a long-term care placement. The five LHINs with the most beds allocated all had the longest wait lists and also the highest number of hospital ALC days.
| LHIN | Number of beds allocated | Total number of ALC days (rank) |
LTC wait list (rank) |
Median time to placement from hospital (rank) |
|---|---|---|---|---|
| Central East | 1,095 | 53,354 (1) | 7,080 (1) | 185 (1) |
| Hamilton Niagara Haldimand Brant | 1,080 | 46,559 (2) | 3,027 (4) | 82 (9) |
| Toronto Central | 1,069 | 30,310 (5) | 2,633 (5) | 113 (6) |
| Central | 1,064 | 35,755 (4) | 4,948 (2) | 153 (2) |
| Champlain | 751 | 37,207 (3) | 3,356 (3) | 98 (8) |
| Mississauga Halton | 649 | 25,412 (7) | 2,300 (6) | 152 (3) |
| North Simcoe Muskoka | 401 | 11,921 (11) | 1,959 (8) | 140 (4) |
| South East | 400 | 20,236 (9) | 1,400 (11) | 80 (10) |
| North East | 384 | 29,470 (6) | 2,040 (7) | 71 (11) |
| South West | 291 | 22,683 (8) | 1,769 (9) | 44 (14) |
| Central West | 266 | 5,687 (14) | 997 (12) | 106 (7) |
| North West | 201 | 18,567 (10) | 817 (13) | 139 (5) |
| Waterloo Wellington | 186 | 10,915 (12) | 1,726 (10) | 70 (12) |
| Erie St. Clair | 52 | 10,243 (13) | 810 (14) | 50 (13) |
As noted above, by 2023-24 the FAO is projecting a 2,000 person increase in the number of Ontarians on the long-term care wait list and a decrease in the median time to placement (from hospitals and the community) from 152 days in 2018-19 to 140 days in 2023-24. However, the FAO projects that the wait time for a long-term care bed will peak at 179 days in 2020-21. This implies that, in the absence of other health sector changes, the problem of hallway health care will get worse over the next two years.
By 2023-24, if all 15,000 new LTC beds have been opened, the wait time for an LTC bed is projected to decline to 140 days. If this improvement in LTC bed wait times also leads to ALC patients spending less time in hospitals waiting for a long-term care bed, then, all else being equal, there could be an improvement in hallway health care by 2023-24 from the LTC bed expansion.
8 | Appendices
Appendix A: LTC Homes Program Spending Details
Long-term care homes program spending has two main channels: level of care (LOC) per diem payments and supplementary payments that reflect provincial priorities.
Level of Care Per Diem Payments
Province
For each day that an LTC home operator has a bed in operation, the operator receives an LOC per diem payment from the Ministry of Long-Term Care through four funding envelopes.[39]
| Category | Description | Per Diem 2019 ($) |
|---|---|---|
| Nursing and Personal Care | Cost of staffing for nursing and personal support services that meet the needs of residents of each particular home | 102* |
| Program and Support Services | Funding for recreational and social activities, medical services, religious practices, etc. | 12 |
| Raw Food | Cost of food (does not include the preparation of food) | 10 |
| Basic Accommodation | Funding for the basic rate of accommodation | 57 |
| Global Increase | Funding that can be applied to any of the four LOC per diem funding envelopes | 2 |
Resident Co-payments
Residents are required to contribute to the cost of accommodation through resident co-payments. All residents are required to pay the basic accommodation rate which is designed to offset the basic accommodation cost paid by the Province to long-term care home operators (see above). However, for low income residents, the Province will cover some or all of the basic rate of accommodation and will reduce the resident’s co-payment.[40]
In addition, residents may choose accommodation in private or semi-private rooms at an additional cost. The added cost for private or semi-private rooms is regulated by the Province and results in additional revenue for long-term care home operators. Overall, monthly rates paid by residents range from $1,891 for basic accommodation to $2,702 for private accommodation.
| Type of Accommodation | Daily Rate | Monthly Rate |
|---|---|---|
| Long-stay basic | $62.18 | $1,891.31 |
| Long-stay semi-private | $74.96 | $2,280.04 |
| Long-stay private | $88.82 | $2,701.61 |
| Short-stay | $40.24 | N/A |
Supplementary Funding
In addition to the LOC per diem payment, there are a number of supplementary funding streams under the long-term care homes program. Many of these funding streams are claims based and can vary from home to home based on the services each long-term care home offers.
| Funding Stream | Description | 2018-19 amount ($ millions) |
|---|---|---|
| Construction Funding Subsidy | Per diem amount provided for new and redeveloped beds subject to a development agreement with MLTC | 150 |
| Physiotherapy | Funded at an annual amount per bed for all homes | 67 |
| Municipal Tax and Allowance Fund | Claims-based reimbursement up to 85% of property tax bill | 63 |
| Behavioural Supports Ontario (BSO) | Amount provided to homes with BSO designation | 58 |
| High Intensity Needs Fund | Claims-based funding to help prevent unnecessary admissions to hospitals and to enable the discharge of patients from hospitals to long-term care | 61 |
| Equalization Adjustment & Pay Equity | Fixed amount subject to pay equity agreement | 126 |
| Resident Assessment Instrument (RAI) | Funding for RAI coordinators that administer the Resident Assessment Instruments. The RAI is a tool used to assess the care needs of long-term care residents. | 40 |
| Other Supplementary Funding Streams |
This includes the following funding streams:
|
198 |
| Total Supplementary Funding | 764 |
Appendix B: Detailed Long-Term Care Homes Program Spending Forecast
| FAO Forecast ($ billions) |
2018-19 | 2019-20 | 2020-21 | 2021-22 | 2022-23 | 2023-24 | Average Annual Growth |
|---|---|---|---|---|---|---|---|
| Nursing and Personal Care | 2.9 | 2.9 | 3.0 | 3.2 | 3.4 | 3.6 | 4.5% |
| Program and Support Services | 0.3 | 0.3 | 0.3 | 0.3 | 0.3 | 0.4 | 5.3% |
| Raw Food | 0.3 | 0.3 | 0.3 | 0.3 | 0.3 | 0.3 | 5.1% |
| Basic Accommodation | 1.6 | 1.6 | 1.7 | 1.8 | 1.9 | 2.0 | 5.0% |
| LOC Per Diem | 5.1 | 5.2 | 5.3 | 5.7 | 6.0 | 6.4 | 4.9% |
| Supplementary Funding Programs | 0.8 | 0.8 | 0.8 | 0.9 | 1.0 | 1.1 | 7.5% |
| Total Cost of Long-Term Care Homes Program | 5.8 | 5.9 | 6.0 | 6.6 | 6.9 | 7.5 | 5.3% |
| Less: Resident Co-payments | -1.5 | -1.6 | -1.6 | -1.7 | -1.8 | -2.0 | 5.0% |
| Net Cost to Province of Long-Term Care Homes Program | 4.3 | 4.4 | 4.4 | 4.9 | 5.1 | 5.6 | 5.4% |
| Number of Beds (end of year) | 78,664 | 78,664 | 79,694 | 85,828 | 88,585 | 93,664 | 3.6% |
| Cost Per Bed Per Day | 149 | 152 | 154 | 158 | 162 | 167 | 2.3% |
Appendix C: Development of this Report
Authority
The Financial Accountability Officer decided to undertake the analysis presented in this report under paragraph 10(1)(b) of the Financial Accountability Officer Act, 2013.
Key Questions
The following key questions were used as a guide while undertaking research for this report:
- What is the current number of long-term care (LTC) beds in Ontario?
- How has the number of LTC beds changed since 2005?
- What is the current wait list for LTC beds in the province?
- How has the wait list changed since 2005?
- Where are individuals on the wait list located (e.g. hospitals, at home, etc.)?
- What is the Province’s benchmark/target for LTC bed wait times?
- How many new LTC beds is the Province expected to create over the next five years?
- What is the estimated cost of the new LTC bed commitment?
- What is the FAO’s projection for the LTC bed waitlist over the next five years given the Province’s new LTC bed commitment?
- What is the FAO’s estimate of LTC bed supply that is required to keep the LTC bed waitlist constant and/or to reduce the LTC bed waitlist?
- What is the per bed cost difference between an individual waiting in a hospital for an LTC bed compared to a resident at an LTC home?
Methodology
This report has been prepared with the benefit of information provided by, and meetings with staff from, the Ministry of Long-Term Care and a review of relevant literature and other publicly available information. Specific sources are referenced throughout.
All dollar amounts are in Canadian, current dollars (i.e. not adjusted for inflation) unless otherwise noted.
The projected long-term care bed wait list is calculated as the difference between the FAO’s projection of long-term care demand and the number of available long-term care beds in Ontario.
Long-term care demand in 2018-19 is estimated based on the number of individuals in long-term care and on the long-term care wait list. The 2018-19 demand was then broken down into five-year age groups and future demand is estimated based on the projected growth of the population in each five-year age group over time using the Ministry of Finance’s “Ontario Population Projections 2018-2046” (updated October 1, 2019). The demand growth in each year is then reduced by 0.54 percentage points to account for an observed trend over time of long-term care demand growth being lower than the growth demographics would indicate.
The number of beds in operation is calculated based on the number of existing beds, and the FAO’s projection of when the 15,000 new beds will be in service, less the number of beds that will be placed in abeyance for redevelopment.
Long-term care wait times are estimated based on an observed relationship between the length of the wait list, the number of beds in operation and the provincial average time to placement.
Footnotes
[1] In addition to funding provided by the ministry through the long-term care homes program, LTC homes also receive payments directly from residents.
[2] Legislative Assembly of Ontario, Hansard, 42nd Parliament, 1st Sess, No 2 (12 July 2018).
[3] 2019 Ontario Budget, p. 117. The 2019 budget also committed to redevelop 15,000 existing long-term care beds to current design standards.
[4] 2019 Ontario Budget, p. 117. See also, FAO, “Expenditure Estimates 2019-20: Ministry of Health and Long-Term Care,” 2019.
[5] The cost of constructing the 15,000 new beds is subsidized by the Province over a 25-year period starting when a new bed comes into service.
[6] Approximately 24 per cent of long-term care residents are placed from hospitals.
[7] See http://www.lhins.on.ca/ for a map of Ontario’s 14 LHINs. LHINs are responsible for planning, funding and delivering health care services to the communities within their networks. In February 2019, the Province announced that it would dissolve the 14 LHINs and consolidate their functions under a new agency, Ontario Health.
[8] Legislative Assembly of Ontario, Hansard, 42nd Parliament, 1st Sess, No 2 (12 July 2018).
[9] 2019 Ontario Budget, p. 117. The 2019 budget also committed to redevelop 15,000 existing long-term care beds to current design standards.
[10] 2019 Ontario Budget, p. 117. See also, FAO, “Expenditure Estimates 2019-20: Ministry of Health and Long-Term Care,” 2019.
[11] Monthly rates paid by residents range from $1,891 for basic accommodation to $2,702 for private accommodation.
[12] The remaining payments made by residents are kept by the long-term care home operators.
[13] Legislative Assembly of Ontario, Hansard, 42nd Parliament, 1st Sess, No 2 (12 July 2018). For the purposes of this report, the FAO interprets the commitment to mean that the 15,000 new beds are intended to be in service by the end of the 2023-24 fiscal year.
[14] Ontario Ministry of Long-Term Care, “Ontario One Step Closer to Creating 15,000 New Long-Term Care Beds,” Oct. 1, 2019.
[15] The ministry states that the information is a Cabinet record that is not authorized to be released under Order in Councils 1002/2018 or 1412/2016.
[16] http://www.health.gov.on.ca/en/pro/programs/ltc/.
[17] Although three years is used as an approximate guideline for the amount of time required from the execution of a development agreement to when a new bed is in service, projects can take considerably longer. Therefore, even if the remaining 7,111 beds are allocated by March 2021, there is no guarantee that all beds will be in service by the end of the 2023-24 fiscal year.
[18] The Ministry of Long-Term Care has provided the FAO with projected timelines for some projects. For those projects the FAO has incorporated the actual project timeline into its forecast. For other projects the FAO assumes a three-year lead time from when the ministry approves a project to when the beds are in service.
[19] There are some exceptions to this statement. For example, not-for-profit or municipal operators are eligible for a planning grant of up to $250,000 that is paid before the beds are in operation.
[20] The amount of the construction funding subsidy is adjusted based on the size of the home and the proportion of basic accommodation beds in the home. See The Province’s Construction Funding Subsidy Policy for more detail.
[21] The construction funding subsidy is a fixed amount provided by the Province that is not intended to cover the full cost of construction. For example, the Conference Board of Canada estimates the capital cost of a long-term care bed to be $320,000 in 2017 dollars. The LTC home operator is responsible for the remaining cost of construction.
[22] See appendix B for a detailed forecast.
[23] The wait list forecast assumes no additional program changes (e.g., expanded community care programming) or long-term care homes program policy changes (e.g., changes to eligibility for the LTC wait list) that could affect long-term care demand.
[24] Ministry of Finance, Ontario Population Projections 2018-2046, updated October 1, 2019.
[25] Statistics Canada, Table 17-10-0005-01. Population estimates on July 1, by age and sex.
[26] Information provided to the FAO by MLTC.
[27] Examples of community-based care include provincially funded home care, care from family members and privately funded retirement homes.
[28] HQO is an agency of the Ministry of Health that acts as the Province’s advisor on health quality.
[29] Health Quality Ontario, “Results from Health Quality Ontario’s Benchmark Setting for Long-Term Care Indicators,” Feb 2017.
[30] Continuing care refers to a range of services that support the health and wellbeing of individuals living in their own home, a supportive living or long-term care setting.
[31] Health Quality Council of Alberta, “Review of Alberta Health Services’ Continuing Care Wait List,” March 2014. This measure has also been recommended to be adopted in British Columbia. See https://bccare.ca/wp-content/uploads/2019/05/Bedlam_in_BC_Continuing_Care_Sector.pdf.
[32] Calgary Herald, “Alberta government missing targets for accessing long-term care,” July 2018.
[33] In 2018-19, approximately 19.1 per cent of Ontarians aged 85 and over were either in long-term care or on the long-term care wait list, compared to 4.2 per cent of Ontarians aged 75 to 84.
[34] The FAO estimates LTC demand growth will accelerate from an annual average of 2.8% from 2018-19 to 2023-24 to 3.6% from 2023-24 to 2033-34.
[35] Assumes no additional program changes (e.g., expanded community care programming) or long-term care homes program policy changes (e.g., changes to eligibility for the LTC wait list) that could affect long-term care demand.
[36] “Hallway Health Care: A System Under Strain,” Premier’s Council on Improving Healthcare and Ending Hallway Medicine, p. 2.
[37] Dr. David Walker, “Caring for Our Aging Population and Addressing Alternate Level of Care,” June 2011.
[38] “Hallway Health Care: A System Under Strain,” Premier’s Council on Improving Healthcare and Ending Hallway Medicine, p. 14.
[39] Effective April 1, 2019, a fifth funding envelope was added to the LOC per diem called the “Global Increase”. LTC homes may allocate up to 32 per cent of the Global Increase funding envelope to the Basic Accommodation envelope. The greater of the remaining balance or 68 per cent of the
Global Increase funding envelope must be applied to the remaining three funding envelopes: Nursing and Personal Care, Program and Support Services, and Raw Food.
[40] See https://www.ontario.ca/page/get-help-paying-long-term-care for more information.


